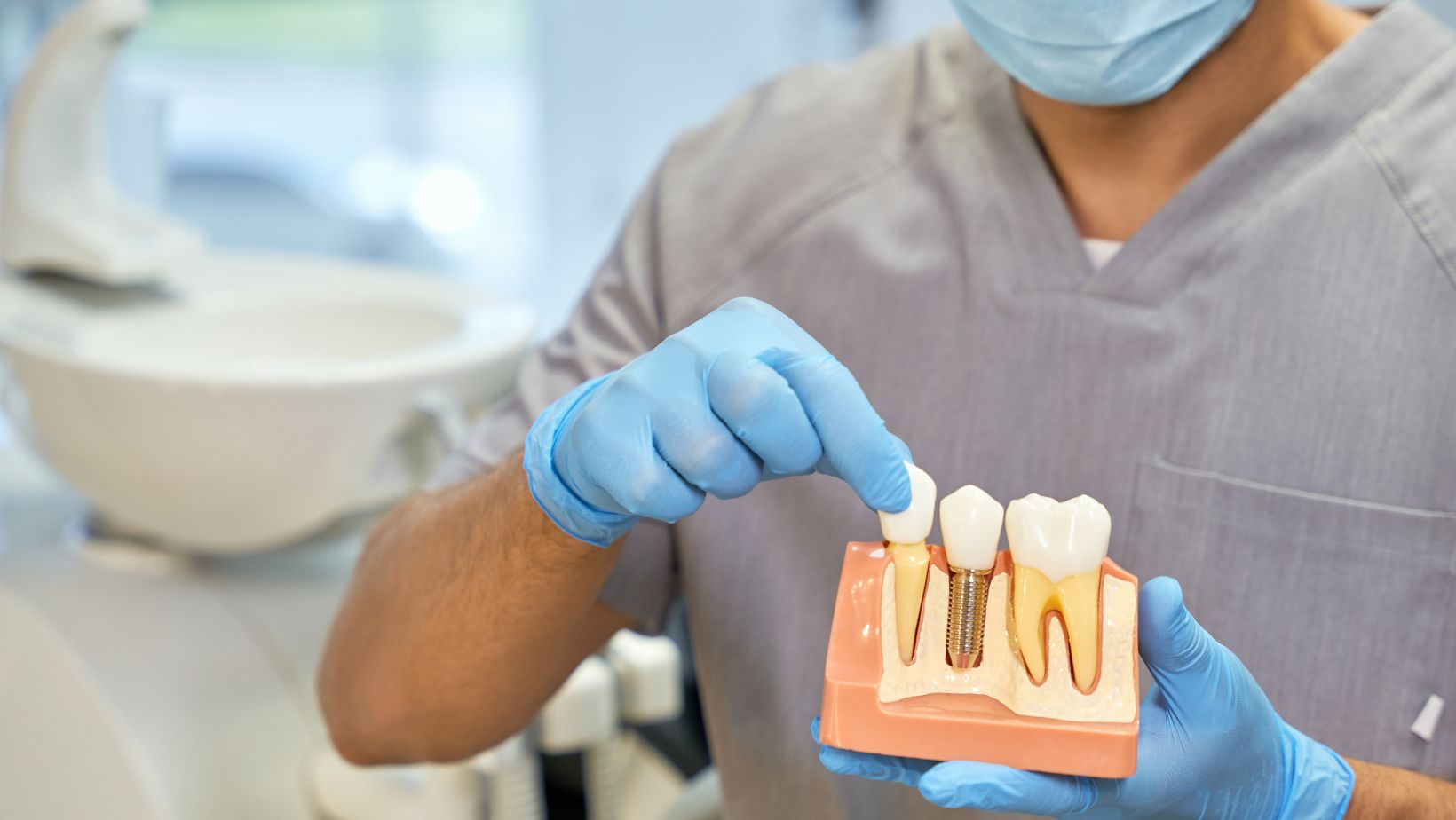
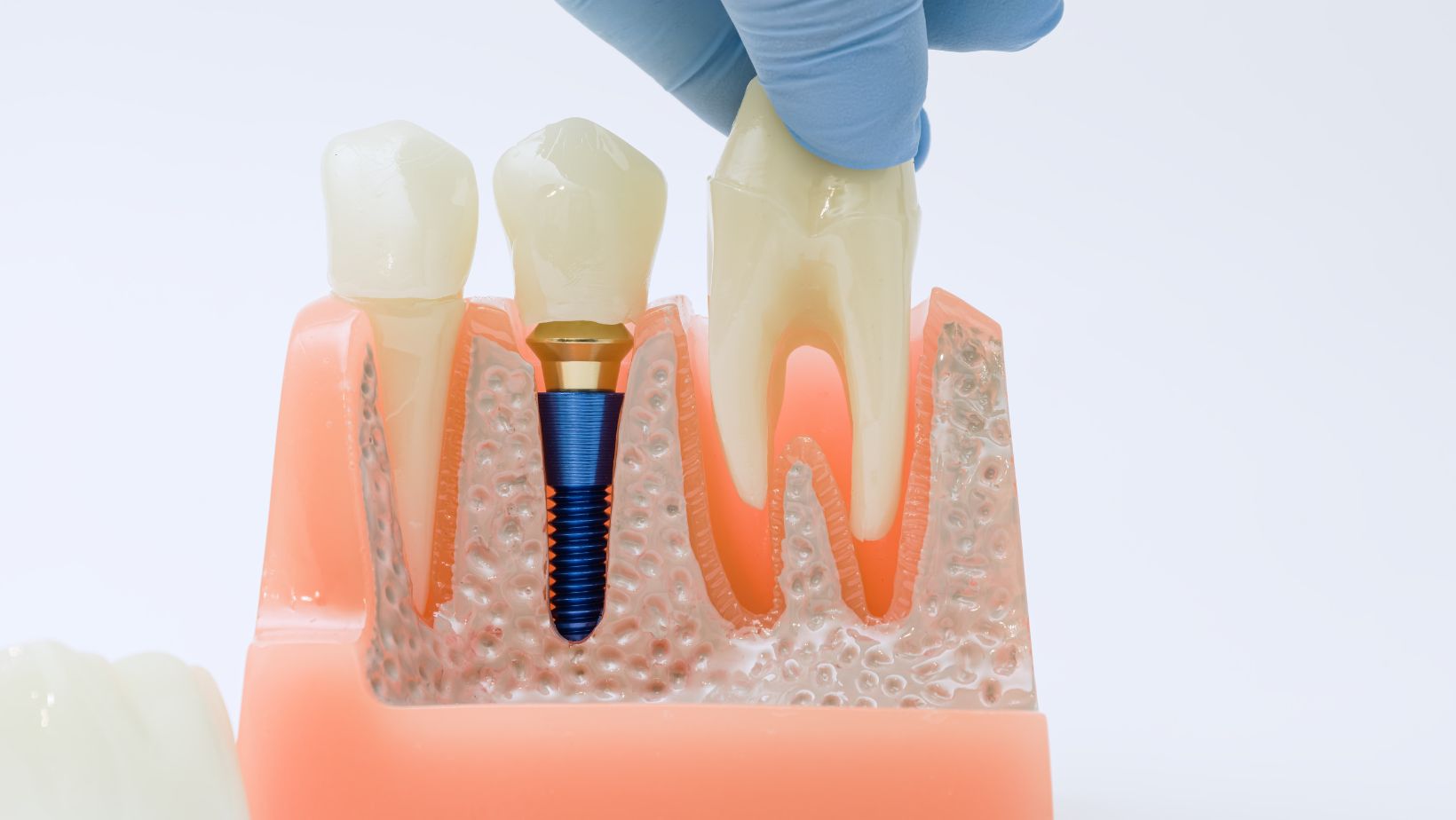
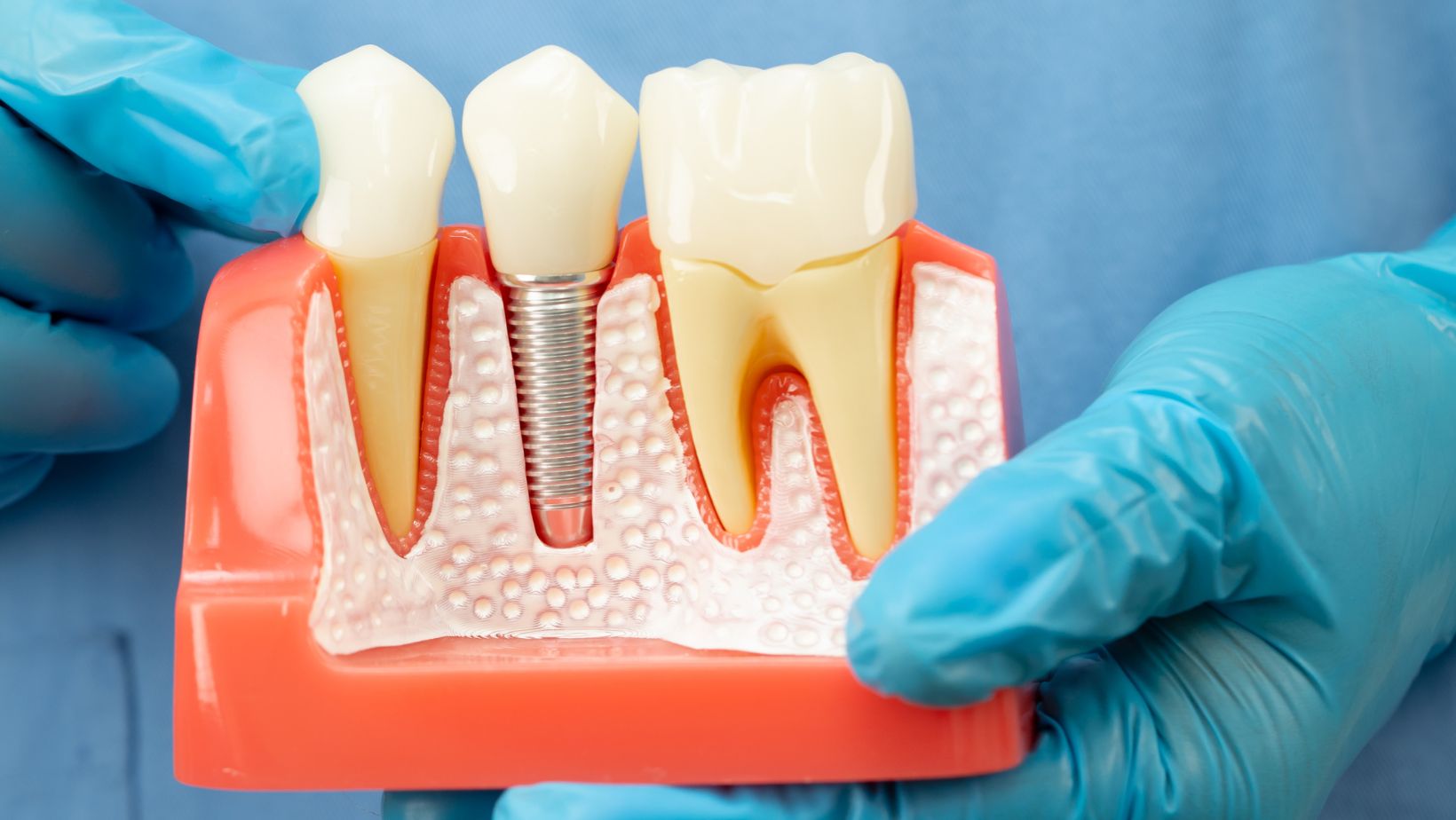
Table of Contents
ToggleDental implants are designed to be reliable, but they can fail in certain situations. The most common causes include poor bone integration, infection around the implant (peri-implantitis), excessive biting forces, or health and surgical complications. Many of these risks can be reduced with thorough planning, proper placement, and consistent aftercare.
If you are considering implants—or already have them—this article explains how failures occur, which warning signs require attention, and what preventive steps help protect your long-term results. You’ll find clear guidance on risk factors, maintenance strategies, and how complications are managed if they arise. When evaluating providers, exploring options for affordable dental implants in Schererville, IN should also include reviewing experience, planning protocols, and follow-up care to ensure long-term success—not just upfront cost savings.
Understanding Dental Implant Failure
You need clear criteria to recognize failure, identify warning signs early, and know the different failure types so you can act quickly and protect your oral health.
Definition of Implant Failure
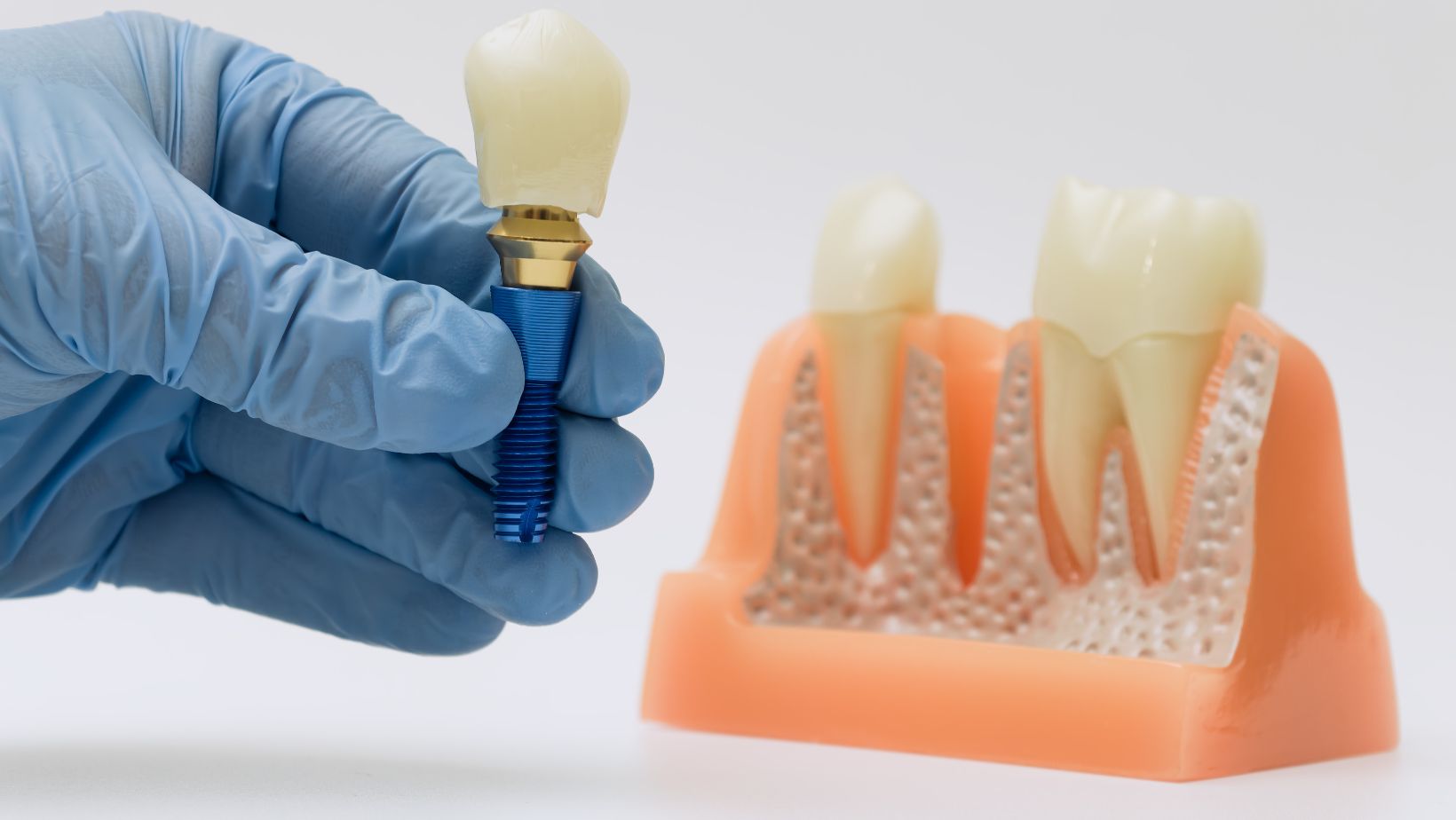
Implant failure occurs when the dental implant loses its stable, functional connection to the jawbone or develops complications that prevent it from performing as intended. Clinically, this often means mobility of the implant, persistent pain, uncontrolled infection, or progressive bone loss visible on radiographs.
Failure can be early (before bone integration) or late (after integration). Early failure usually reflects surgical issues, poor bone quality, or healing problems. Late failure most often stems from infection around the implant, excessive mechanical load, or systemic health factors that degrade bone support.
Symptoms and Early Warning Signs
Watch for persistent pain that doesn’t subside after the normal healing period of several weeks. New or worsening mobility of the implant, swelling, pus discharge, or a bad taste/smell in your mouth indicate infection.
Gum bleeding around the implant, recession exposing part of the implant, and increasing sensitivity or difficulty chewing are important early signs. Changes on follow-up X-rays—such as bone loss around the implant—often precede obvious symptoms, so attend scheduled radiographic checks.
Types of Implant Failure
- Early (Primary) Failure: Occurs before osseointegration; common causes include surgical trauma, inadequate primary stability, contamination during placement, or compromised bone quality.
- Late (Secondary) Failure: Happens after initial integration; typical causes are peri-implantitis (bacterial infection with bone loss), overload from bruxism or poorly designed restorations, and systemic conditions like uncontrolled diabetes.
- Mechanical Failure: Involves broken components (screws, abutments) or prosthetic complications that compromise function without immediate bone loss.
- Biological Failure: Driven by infection or bone resorption leading to loss of bone support and implant loosening.
For each type, timely diagnosis guides management: early failures may need removal and possible reimplantation, mechanical issues often require component repair, and biological failures require infection control plus bone therapy.
Primary Causes of Dental Implant Failure
You should understand the main reasons implants can fail so you can spot risks and take prevention steps. These causes include bone problems, hygiene lapses, infections around the implant, and medical conditions that impair healing.
Insufficient Bone Quality or Quantity
If your jaw lacks adequate bone height, width, or density, the implant may not achieve or keep stable integration with the bone (osseointegration). Common causes include long-standing tooth loss, advanced periodontal disease, or trauma that reduced bone volume.
Your dentist will evaluate bone with CBCT or periapical radiographs before placement. When bone is insufficient, predictable options include bone grafting, sinus lift (upper posterior maxilla), or selecting narrower/shorter implants—each choice affects healing time and success probability.
Smoking and untreated systemic conditions worsen bone remodeling and graft outcomes. Expect a longer treatment timeline and additional procedures if your clinician recommends augmentation to create a stable foundation for the implant.
Poor Oral Hygiene
Plaque accumulation around an implant leads to inflammation that undermines the soft tissue seal and bone support. Brushing alone may not remove interdental plaque; you must use floss, interdental brushes, or water flossers targeted to the implant crown and abutment junction.
Missed professional cleanings accelerate progression from mucositis (reversible soft tissue inflammation) to bone-loss conditions. Your implant prosthesis design matters: poorly contoured crowns or tight embrasures can trap food and make cleaning difficult, increasing failure risk.
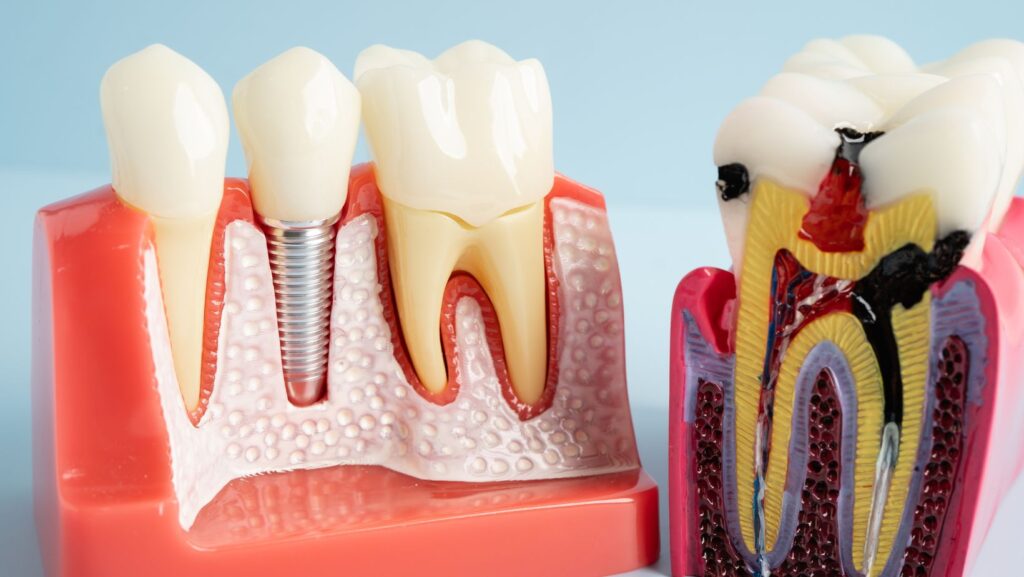
Follow a schedule of twice-yearly or more frequent maintenance visits if you have risk factors. Your dental team can show specific home-care techniques and adjust the prosthesis to improve access for cleaning.
Peri-Implantitis and Infection
Peri-implantitis presents as bleeding on probing, progressive bone loss, and sometimes suppuration around the implant. It results from bacterial colonization and an unchecked host inflammatory response; it differs from surgical-site infection that may happen immediately post-op.
Early detection matters: look for bleeding, increased probing depths, mobility, or exposed threads. Treatment ranges from nonsurgical debridement with adjunctive antiseptics or local antibiotics to surgical access, bone regeneration, or implant removal in severe cases.
Risk factors include prior periodontitis, poor hygiene, smoking, and residual cement left under restorations. Preventive steps include meticulous restorative margins, routine monitoring with radiographs, and immediate management of any soft-tissue inflammation.
Medical Conditions Impacting Healing
Systemic diseases and medications can impair bone healing and immune response, raising failure risk. Diabetes with poor glycemic control, osteoporosis treated with certain antiresorptives, uncontrolled autoimmune disease, and radiotherapy to the head and neck are notable examples.
Tell your dentist about conditions and medications—including bisphosphonates, denosumab, corticosteroids, and immunosuppressants—so they can modify timing, surgical technique, and follow-up. For diabetes, aim for stable HbA1c targets before elective implant surgery to reduce complications.
Collaborative care with your physician may include temporary medication adjustments, antibiotic prophylaxis, or delaying treatment until medical status improves. Your individualized risk assessment guides whether implants remain a safe option and what precautions to take.
Prevention Strategies for Long-Term Success
You can significantly reduce implant failure risk by thorough assessment, precise surgery, careful aftercare, and lifestyle changes. Each step targets specific failure causes like poor bone integration, infection, or excessive mechanical load.
Pre-Operative Assessment and Planning
Start with a comprehensive medical and dental history review. Tell your clinician about diabetes, osteoporosis, smoking, radiation therapy, or medications (bisphosphonates, immunosuppressants) because these affect bone healing and infection risk.
Get a CBCT or panoramic radiograph to evaluate bone volume, density, and anatomical landmarks. Your surgeon should measure available bone height and width, assess sinus proximity and nerve location, and plan implant size and angulation accordingly.
Consider preparatory treatments when needed. Bone grafting, sinus lift, periodontal therapy, or staged extractions improve the local environment for osseointegration. Discuss realistic timelines and success rates based on your specific anatomy.
Surgical Technique and Expertise
Choose a clinician with documented implant training and a track record of similar cases. Experience reduces surgical complications and improves prosthetic outcomes.
Insist on sterile technique and use of appropriate instruments and implant systems. Atraumatic flap handling, precise osteotomy, and controlled insertion torque protect bone and minimize microfracture that can impair integration.
Follow implant-specific protocols for immediate vs. delayed loading. Your surgeon should decide loading time based on primary stability (insertion torque or implant stability quotient). If stability is low, delay loading and use a healing cap or temporary prosthesis.
Post-Operative Care
Follow prescribed antibiotics, analgesics, and any chlorhexidine rinses exactly as directed. These reduce early infectious complications and help soft tissue healing.
Maintain gentle oral hygiene around the site for the first two weeks, then resume normal cleaning using a soft-bristled brush and interdental tools. Attend scheduled follow-ups at 1 week, 1 month, and completion of prosthesis, and any additional visits your clinician recommends.
Report fever, increasing pain, pus, persistent bleeding, or implant mobility immediately. Early intervention—debridement, antibiotics, or removal—limits bone loss and preserves options for future rehabilitation.
Lifestyle Modifications
Stop smoking before surgery and continue abstinence during healing. Smoking impairs blood flow and doubles the risk of implant failure in many studies.
Control systemic conditions proactively. Keep blood glucose within target ranges if you have diabetes, optimize bone health through vitamin D and calcium intake, and review medications with your provider if they affect bone metabolism.
Protect implants from excessive force. If you grind or clench, get a nightguard. Avoid chewing hard items (ice, nutshells) on the implant restoration. Address parafunctional habits early to prevent mechanical overload and component failure.
Managing and Addressing Implant Complications
You can take specific steps to limit damage and restore function when problems arise. Timely action, targeted treatments, and scheduled checks are the pillars of managing implant complications.
Early Intervention Approaches
Act quickly at the first sign of pain, swelling, bleeding, mobility, or a bad taste. Early visits let your clinician diagnose issues like peri-implant mucositis, infection, or occlusal overload before bone loss occurs.
Common early measures include:
- Mechanical debridement of the implant surface to remove plaque and biofilm.
- Topical or systemic antibiotics when bacterial infection is confirmed or spreading.
- Adjustment of occlusion to reduce excessive forces that can loosen components.
- Soft-tissue management (local antiseptics, improved oral hygiene instruction) to reverse mucositis.
You should expect short-term re-evaluation within 1–2 weeks after therapy and radiographic checks if symptoms persist. Early, conservative care often prevents progression to bone loss and implant failure.
Revision Procedures
If conservative care fails or bone loss is significant, your dentist may recommend surgical revision or implant removal. The chosen procedure depends on cause, extent of bone loss, and your overall health.
Revision options:
- Surgical flap and debridement with implant surface decontamination for peri-implantitis.
- Bone grafting and guided bone regeneration (GBR) to rebuild lost alveolar bone if conditions allow re-implantation.
- Implant removal followed by socket preservation when the implant is non-salvageable.
- Replacement with a new implant or alternative prosthesis after adequate healing and risk modification.
Plan for staged treatment: resolve infection first, restore bone and soft tissue next, then consider re-implantation. Expect multiple visits, possible temporary prosthesis, and longer healing times after revision surgery.
Monitoring and Regular Follow-Ups
After any treatment, schedule systematic follow-ups to detect recurrence early and protect long-term success. Your follow-up plan should include clinical exams, radiographs, and hygiene reinforcement.
A typical schedule:
- Post-op checks at 1–2 weeks, 3 months, and 6 months in the first year.
- Annual clinical and radiographic assessments thereafter, more frequent if risk factors exist (smoking, diabetes, history of periodontitis).
During visits, your clinician will measure probing depths, check for bleeding on probing, evaluate prosthetic fit, and compare radiographs to prior images. Maintain meticulous home care and attend professional cleanings every 3–6 months if you have risk factors.