Table of Contents
ToggleYou can care for dental implants much like natural teeth: brush daily, clean between teeth consistently, attend regular professional checkups, and manage lifestyle factors such as smoking and diet to protect gum and bone health. Strong home care combined with routine dental visits keeps implants stable, lowers infection risk, and extends their lifespan.
You will find practical guidance on brushing and flossing techniques designed specifically for implants, recommended tools, and what your dental team monitors during follow-up visits. You will also learn which habits protect or shorten implant longevity so you can make informed decisions that safeguard your investment. If cost is part of your concern, exploring options for affordable dental implants can help you balance long-term durability with a treatment plan that fits your budget.
Daily Oral Hygiene for Dental Implants
Maintain mechanical removal of plaque, protect peri-implant tissue, and use products that won’t scratch implant surfaces. Small technique changes and the right tools prevent inflammation and extend the life of your implants.
Brushing Techniques for Implants
Use a soft-bristled or specifically designed implant toothbrush and brush twice daily for at least two minutes. Hold the brush at a 45° angle where the crown meets the gum to dislodge plaque at the margin, and use gentle circular motions rather than aggressive back-and-forth scrubbing.
If you have a bridge or multiple adjacent implants, clean along the gumline and the prosthesis base; short strokes help reach tight areas. Electric toothbrushes with pressure sensors reduce overbrushing and improve plaque removal — choose one with a small head for better access.
Rinse after brushing if you use a fluoride or antimicrobial rinse, but avoid vigorous swishing that can irritate healing tissue. Replace your brush or brush head every 3 months or sooner if bristles fray.
Flossing Around Implant Sites
Use implant-safe floss or a floss threader to pass floss beneath the prosthetic contact and along the implant-abutment interface. Slide the floss gently up and down against the side of each implant crown and beneath the contact to remove biofilm without forcing floss into the sulcus.
Consider interdental brushes with soft, non-metallic coatings for wider spaces; choose sizes that fit without bending the wire against the implant surface. Water flossers can effectively flush debris from around implants—use a low-to-medium pressure setting and aim the nozzle at a 45° angle into the sulcus.
Perform interdental cleaning once daily, ideally before bedtime, when saliva flow is reduced and plaque removal matters most. If you notice bleeding, persistent swelling, or discomfort, contact your dentist for assessment.
Selecting Appropriate Dental Products
Select non-abrasive fluoride toothpaste labeled for sensitive or daily use to avoid scratching ceramic or metal implant surfaces. Avoid highly abrasive whitening pastes and baking soda-based products that can dull the prosthesis finish.
Choose interdental brushes with nylon or rubber-coated bristles and avoid exposed metal wires that could abrade implants. Pick an antimicrobial rinse (chlorhexidine short-term or alcohol-free essential-oil rinses for routine use) only under guidance if you have peri-implant inflammation.
Electric toothbrushes with soft brush heads, pressure sensors, and small brush heads work best. Replace or sterilize tools per manufacturer guidance, and bring your products to follow-up visits so your dentist can recommend any adjustments.
Professional Dental Care and Maintenance
You should expect regular professional oversight, targeted cleanings, and specific checks that track implant stability and surrounding bone. These appointments prevent problems early and keep your implants functioning like natural teeth.
Routine Dental Checkups
Attend checkups at least every six months, or more often if your dentist recommends it based on your risk factors. During visits your clinician will review your medical history, inspect the soft tissues, and assess how your implant crown and neighboring teeth are wearing.
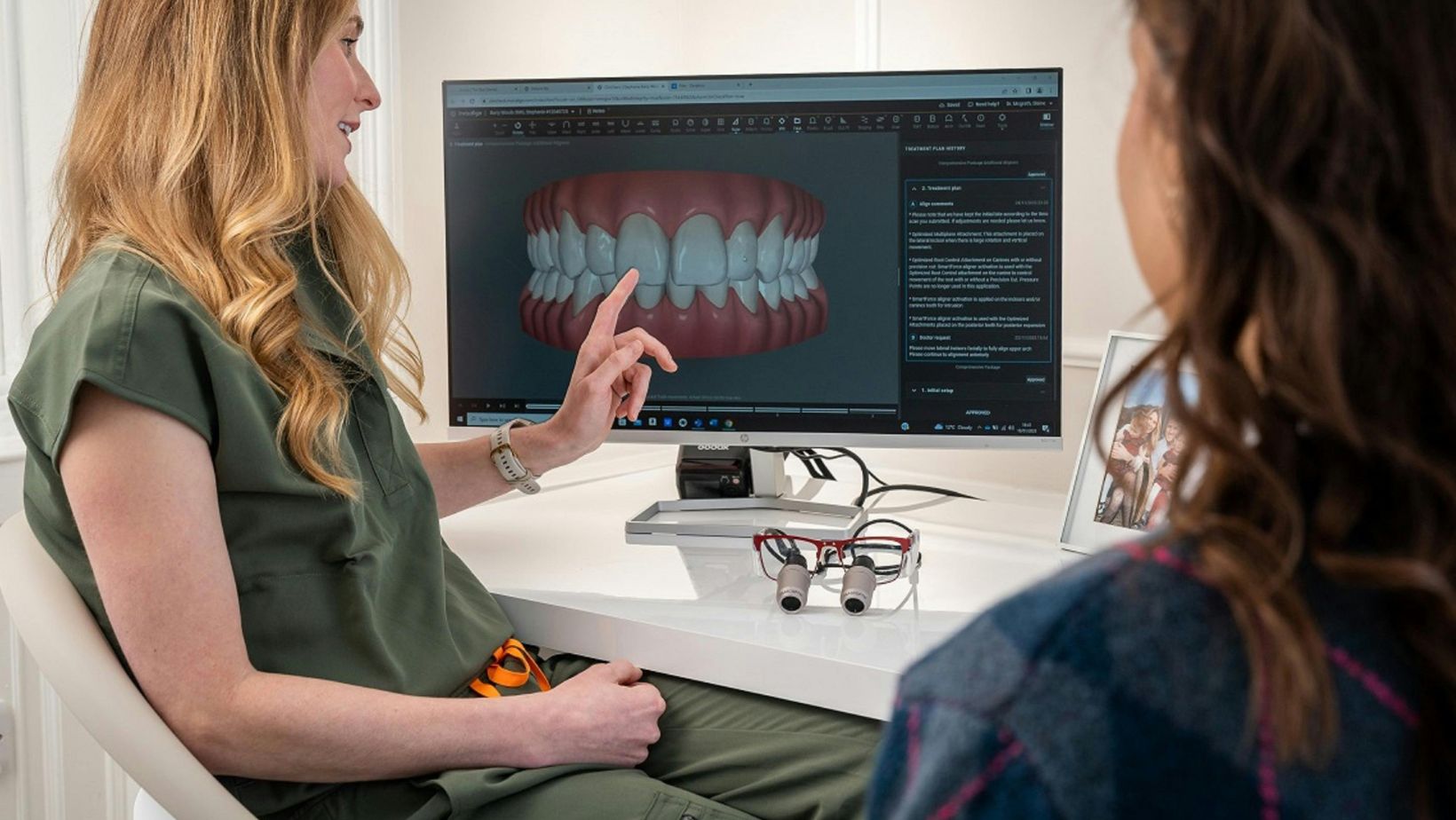
Expect periodic X-rays—usually periapical or panoramic—to measure bone levels around the implant and detect any hidden bone loss. Your dentist will also check the implant-abutment connection for tightness and evaluate your bite to prevent undue forces that can loosen components.
Bring up any sensitivity, loosening, or bleeding you notice between visits. Early reporting lets your provider address issues such as peri-implant mucositis before they progress.
Professional Cleaning Procedures
Professional cleanings use instruments that avoid scratching implant surfaces; your hygienist will use plastic, resin, or specially coated metal scalers and ultrasonic tips approved for implants. These tools remove plaque and calculus without damaging the implant’s surface or the crown margins.
Expect targeted polishing and irrigation around the implant to reduce bacterial load. Your hygienist may apply antimicrobial rinses or localized antibiotic therapy if inflammation is present.
If you have hard-to-reach areas, the team will teach and demonstrate techniques and tools—interdental brushes, floss threaders, or water flossers—so you can maintain plaque control at home between professional cleanings.
Monitoring Implant Health
Your dentist will document pocket depths around the implant and compare measurements over time. Stable, shallow pockets generally indicate healthy tissue; increasing depth signals the need for intervention.
Watch for signs your clinician will track: persistent bleeding on probing, suppuration, increased mobility, or radiographic bone loss. If peri-implantitis is suspected, your provider will outline staged treatment options such as mechanical debridement, antimicrobial therapy, and possible surgical intervention.
Keep a log of symptoms and appointment outcomes. Consistent records help your dental team detect trends and tailor maintenance intervals or additional treatments to protect the implant long term.
Lifestyle Factors Impacting Implant Longevity
Your daily choices—what you eat, behaviors you avoid, and how you manage health conditions—directly affect how long implants last. Small, consistent actions like avoiding hard foods, quitting smoking, and controlling blood sugar make measurable differences.
Diet and Nutrition Considerations
Focus on a balanced diet that supports bone and gum health. Eat calcium-rich foods (low-fat dairy, fortified plant milks, leafy greens) and foods high in vitamin D and K to support bone remodeling around the implant. Include lean protein and vitamin C sources (citrus, bell peppers, strawberries) to support tissue repair and immune function.
Limit very hard, sticky, or chewy items that concentrate force on a single implant crown; avoid biting whole nuts, hard candy, or ice. Reduce frequent sugary snacks and acidic beverages to lower risk of peri-implant inflammation and soft-tissue irritation. Stay hydrated and consider a calcium + vitamin D supplement only if your dentist or physician recommends it based on labs or dietary gaps.
Avoiding Harmful Habits
Smoking and tobacco use increase implant failure risk by impairing blood flow and wound healing. If you currently smoke or vape, quitting or cutting back before surgery and during healing improves osseointegration and long-term success.
Avoid chronic teeth grinding (bruxism) or use a night guard if you clench; occlusal overload can loosen implants or damage prosthetics. Don’t use implants as tools—open packages or bite nonfood objects—and avoid repetitive chewing of hard pens or fingernails. Limit alcohol intake during healing, as heavy drinking can delay tissue repair and weaken immune response.
Managing Chronic Health Conditions
Control diabetes tightly; high blood glucose raises infection risk and slows healing around implants. Work with your physician to keep HbA1c in target range before and after implant placement, and follow prescribed medications and wound-care instructions closely.
Address periodontal disease before implant surgery and maintain regular professional cleanings afterward to prevent peri-implantitis. If you take medications that affect bone metabolism (bisphosphonates, denosumab) or immunosuppressants, inform your dentist and physician—treatment timing and risk mitigation strategies may change. Keep routine medical and dental appointments so providers can monitor healing and intervene early if problems arise.