Table of Contents
ToggleWorried that getting a dental implant will mean days of severe pain? Most people experience only mild to moderate discomfort that you can manage with short-term pain relievers and simple aftercare.
You will learn what happens during the procedure, how patients typically feel right after surgery, and practical steps you can take to minimize soreness and speed healing. The article draws on typical patient reports and current practice so you can decide with confidence what to expect.
What to Expect During Dental Implant Procedures
You will experience a planned sequence of steps, active pain control, and choices about anesthesia or sedation. Expect local numbness during the procedure, short-term soreness afterward, and tailored medications or techniques to keep you comfortable.
Step-by-Step Overview of Implant Placement
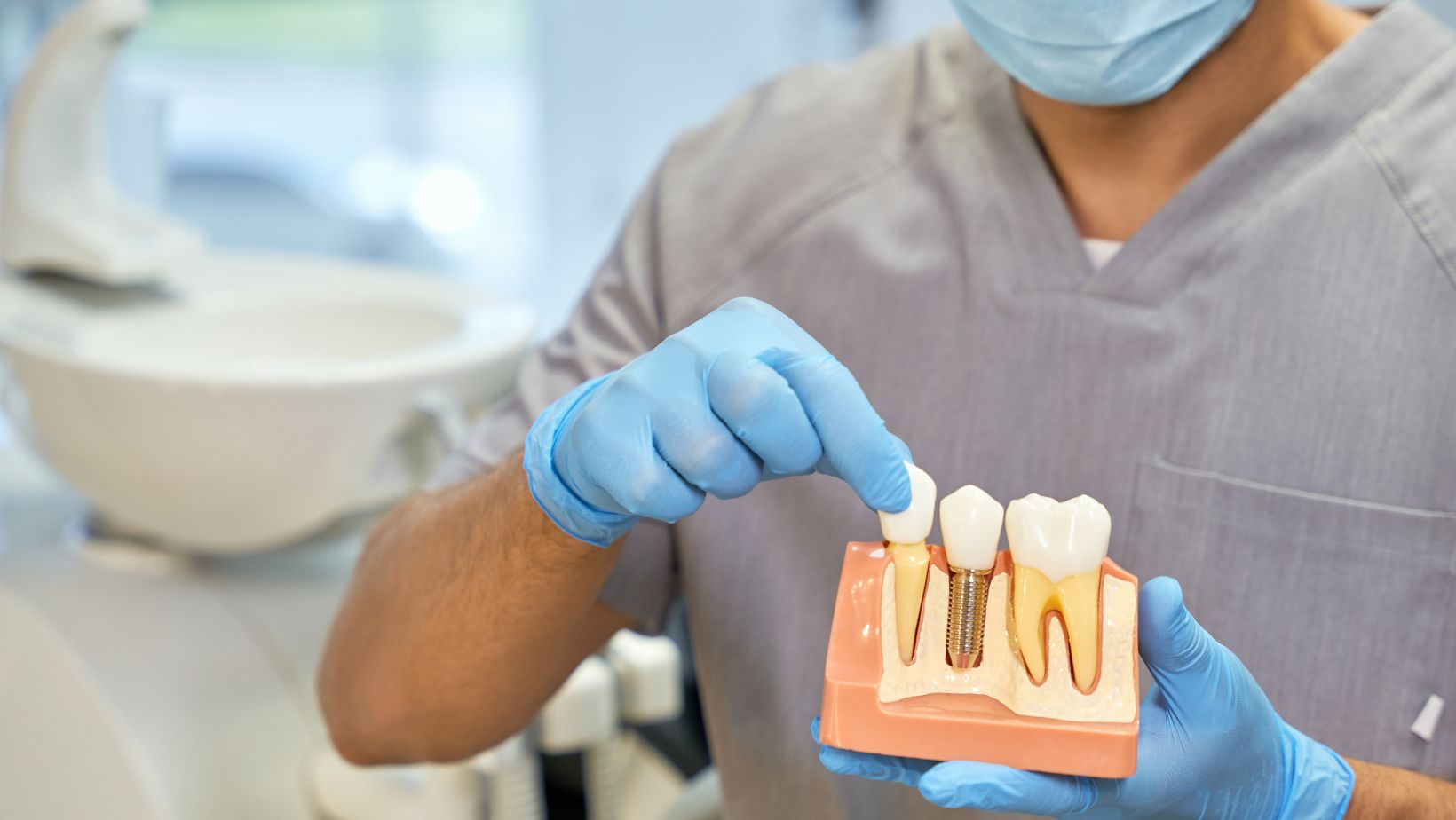
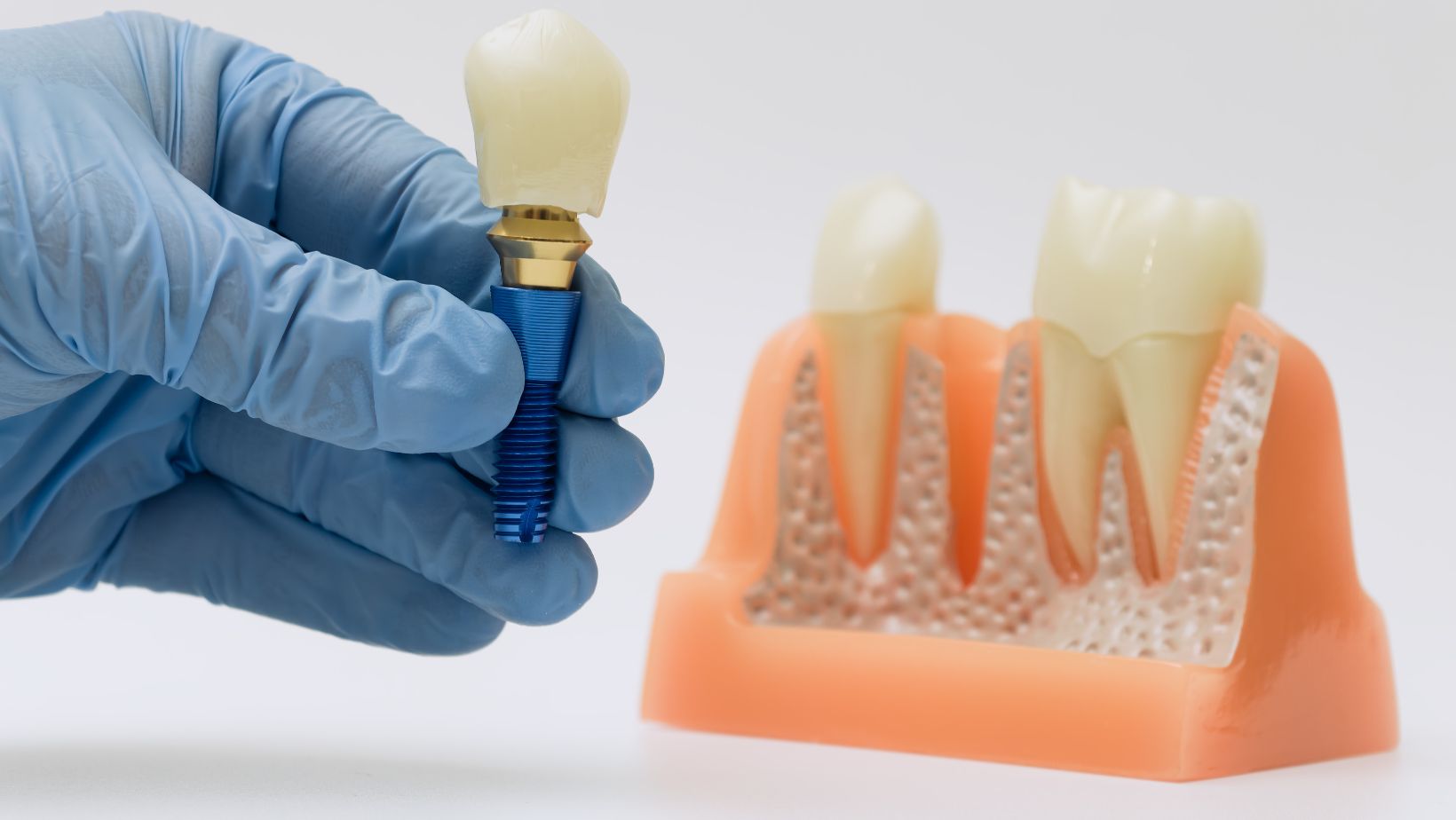
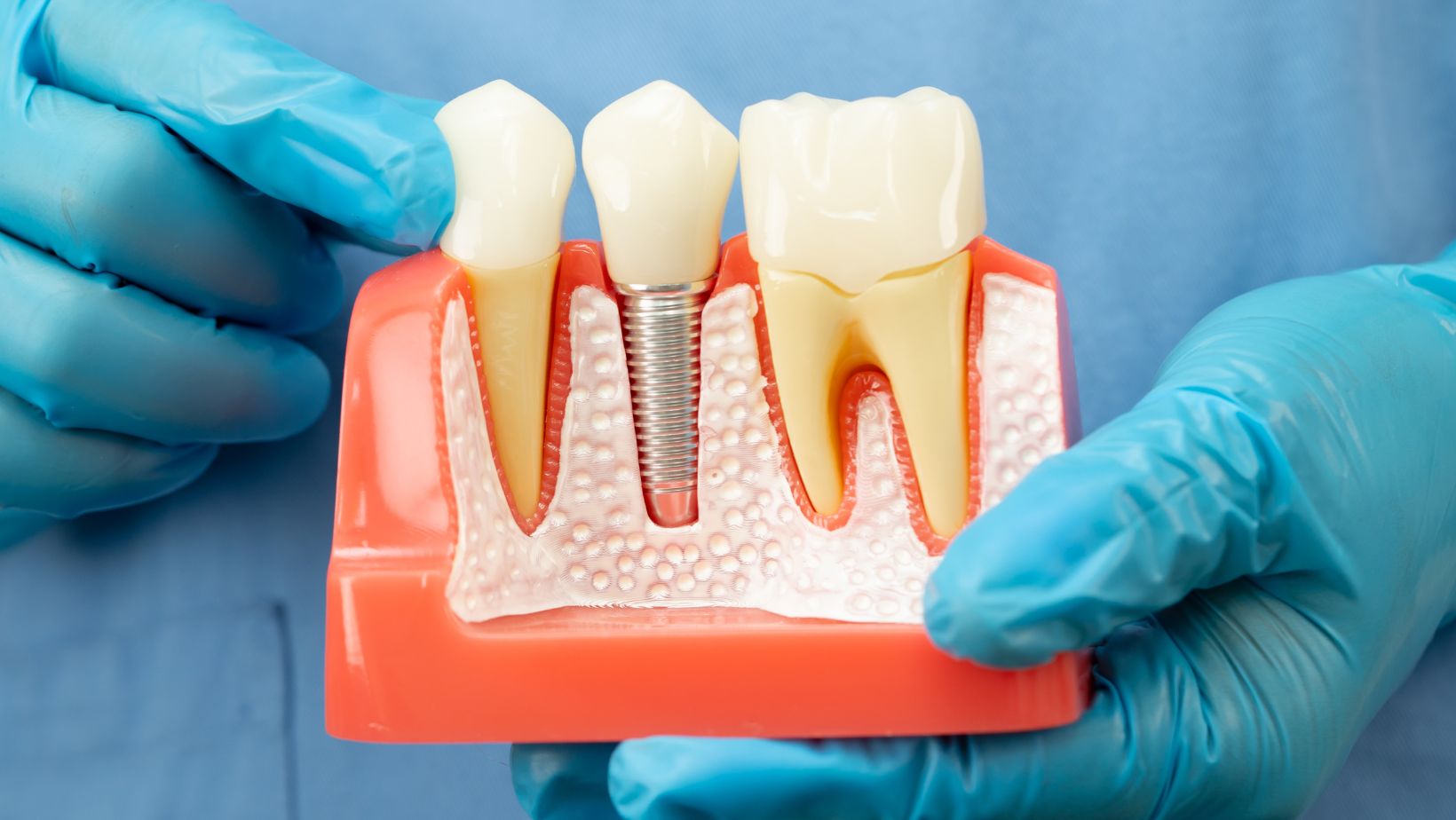
Your visit usually begins with a clinical exam and imaging (CBCT or panoramic X-ray) to map bone and nerve locations. Your dentist or oral surgeon makes a small incision in the gum, exposes the bone, and drills a precise osteotomy (hole) sized for the implant screw.
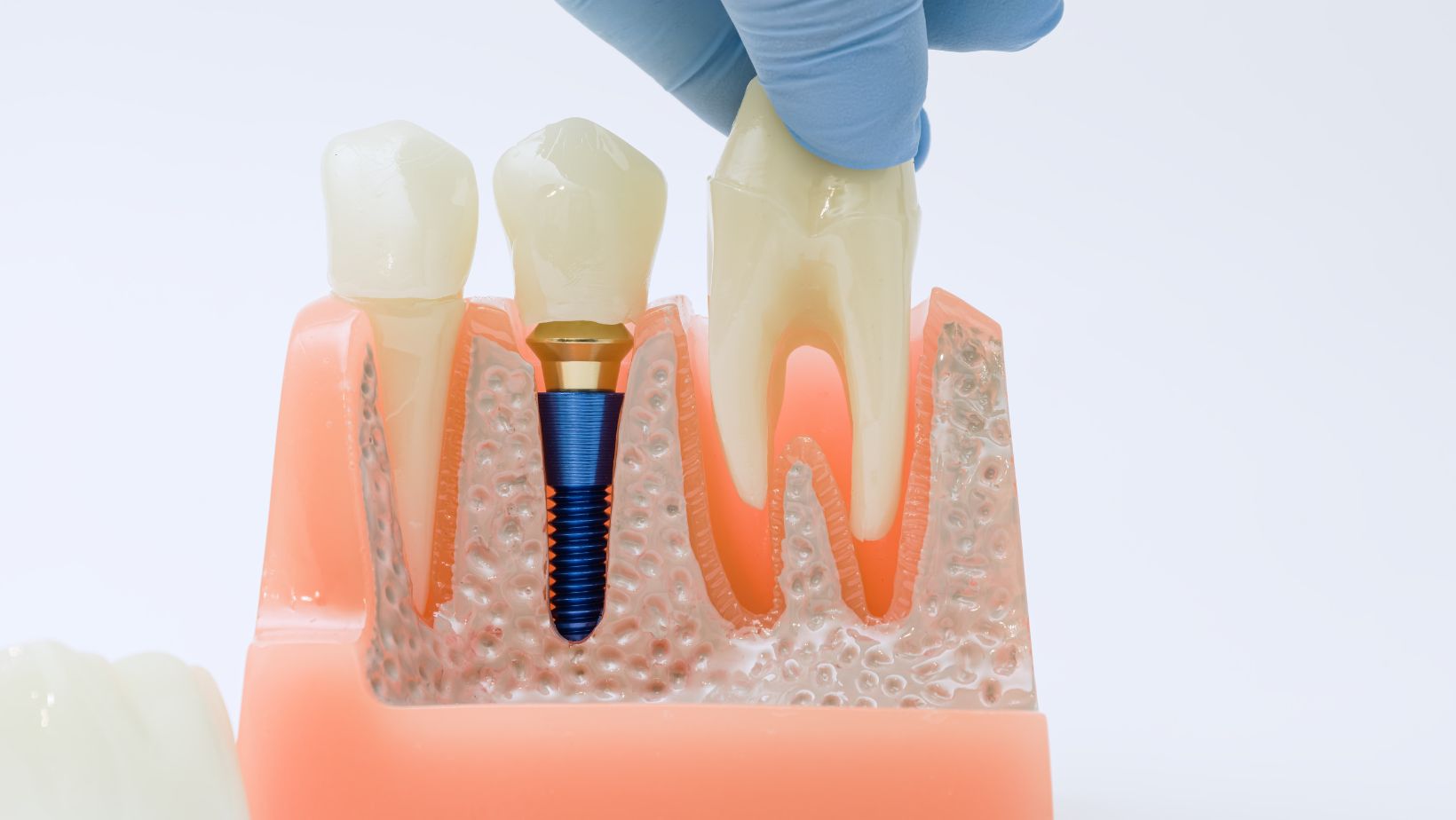
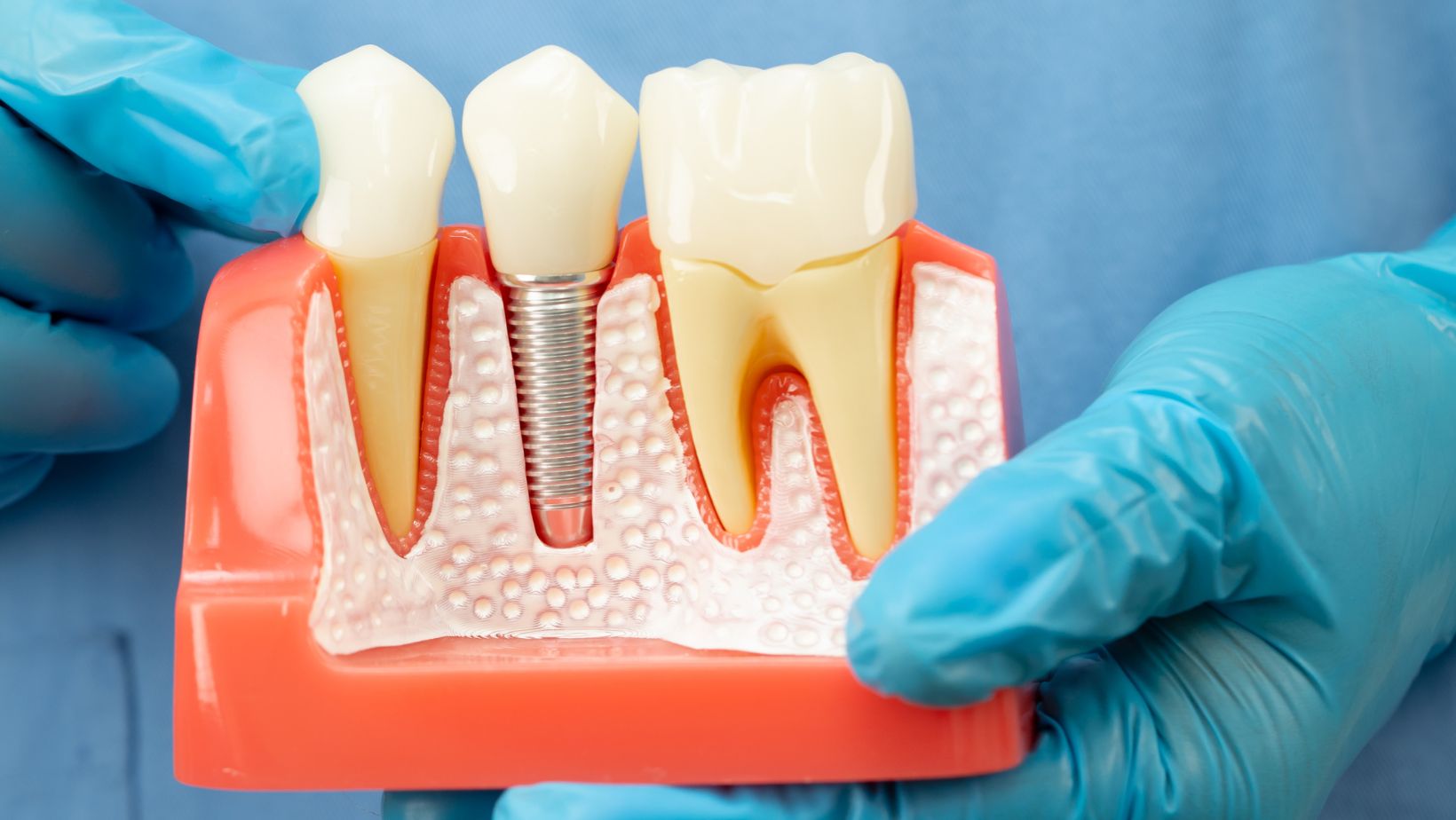
The dental implant (a titanium or titanium-alloy post) is placed into the bone and may receive a healing cap or a temporary crown. If bone grafting or sinus lift is needed, that can be done at the same visit or staged earlier. The wound is sutured, and you leave with written aftercare instructions and a schedule for follow-up.
Osseointegration (bone fusing to the implant) takes several weeks to months. After sufficient healing, your provider uncovers the implant if buried, takes impressions, and fits the final abutment and crown.
Pain Management Techniques Used by Dentists
Dentists use layered pain control: local anesthesia for the procedure, prescription or over-the-counter analgesics afterward, and topical anesthetics for injection comfort. They often recommend ibuprofen (or naproxen) as first-line for inflammation-related pain, sometimes combined with acetaminophen for additive effect.
For moderate-to-severe discomfort, short courses of prescription opioids are rare but available. Ice packs applied to the cheek for 24–48 hours reduce swelling and pain. Clear postoperative instructions — soft diet, avoid smoking, and gentle oral hygiene — minimize complications that would increase pain.
If you have anxiety, providers add sedation to reduce stress and perceived pain. They tailor medication choices to your health, allergy profile, and interaction with other prescriptions.
Types of Anesthesia and Sedation Options
Local anesthesia (e.g., lidocaine with epinephrine) numbs the surgical site and is standard for implant placement. You remain awake and responsive with no systemic drowsiness, and the injection itself may be softened with topical numbing gel.
Conscious sedation options include oral sedatives (e.g., triazolam or diazepam), nitrous oxide (laughing gas), and IV sedation (propofol or midazolam administered by a trained clinician). These reduce anxiety and memory of the procedure but require monitoring and sometimes a companion for transportation.
General anesthesia is rarely used for routine single-implant cases but may be offered for complex, multiple implants or medically anxious patients. Your clinician reviews risks, fasting rules, and post-anesthesia recovery steps before choosing the appropriate option.
Patient Experiences With Dental Implant Pain
Most patients report manageable soreness, predictable swelling, and brief nerve sensitivity. You can expect pain to peak early, respond to common painkillers, and taper over days to weeks depending on the procedure and your health.
Common Sensations Reported After Surgery
You will feel local soreness at the implant site that patients rate about 2–4/10 on typical pain scales. The jaw and gum around the implant often ache rather than throb sharply.
Expect moderate swelling and bruising for 48–72 hours. Chewing near the area will feel awkward; stick to soft foods to avoid pressure.
Nerve-related sensations such as tingling or numbness sometimes occur if a nearby nerve was irritated; these usually improve but should be reported if persistent.
Mild bleeding or oozing during the first day is common. If you experience severe, increasing pain or heavy bleeding, contact your dentist promptly.
Realistic Recovery Timeline
Day 0–3: Pain usually peaks within the first 48–72 hours. You’ll likely take prescription or over-the-counter pain medicine during this window. Rest and ice reduce swelling.
Day 4–14: Discomfort typically decreases each day. By one week many patients feel only mild soreness and can return to normal activities. Stitches, if present, often dissolve or come out in this period.
Weeks 3–12: Bone integration (osseointegration) continues with little pain, though you may feel occasional sensitivity when chewing. Most patients report being functionally comfortable by 2–3 weeks and pain-free by 2–3 months, depending on complexity.
Individual Factors Influencing Discomfort
Procedure complexity changes outcomes: single implants with no grafting cause less pain than multiple implants or bone grafts. If your surgeon performed sinus lifts or significant grafting, expect a longer, more uncomfortable recovery.
Medical status matters. Smoking, uncontrolled diabetes, and certain medications (like bisphosphonates) slow healing and can increase pain or complications. Tell your dentist about all medications and conditions.
Pain tolerance and anxiety affect your perception; high anxiety can heighten reported pain. Follow pre- and post-op instructions—medication schedule, oral hygiene, and diet—to reduce discomfort and speed healing.
Minimizing and Managing Pain After Dental Implants
You can significantly reduce discomfort by following specific aftercare steps, taking the right medications, and knowing clear signs that need professional attention. Practical actions in the first 72 hours make the biggest difference.
Recommended Aftercare Practices
Use a cold compress on the outside of your cheek for 15 minutes on, 15 minutes off during the first 24 hours to limit swelling and reduce pain. Keep your head elevated while resting to minimize blood flow to the area.
Rinse gently with warm salt water (1/2 teaspoon salt in 8 oz water) starting 24 hours after surgery, four times daily and after meals. Avoid vigorous swishing, spitting, or using alcohol-based mouthwash for at least one week to protect the surgical site.
Stick to a soft-food diet for 7–10 days: mashed potatoes, yogurt, scrambled eggs, and smoothies (avoid straws). Chew on the opposite side of the implant and cut food into small pieces to prevent stress on the implant area.
Keep oral hygiene meticulous but gentle. Brush adjacent teeth normally; use a soft-bristled brush near the implant and avoid brushing the incision directly for 3–5 days. Follow any specific instructions your surgeon gives about temporary sutures or chlorhexidine rinses.
Avoid smoking, heavy exercise, and alcohol for at least 72 hours. These activities increase bleeding risk, delay healing, and can intensify pain.
Medications Commonly Prescribed
Your clinician will often prescribe a short course of antibiotics if they assess infection risk; take the full course even if you feel better. Common choices include amoxicillin or, for penicillin-allergic patients, azithromycin or clindamycin.
For pain control, dentists typically recommend over-the-counter NSAIDs such as ibuprofen (200–400 mg every 4–6 hours as needed, not exceeding 2400 mg/day) because they reduce inflammation and pain. Acetaminophen (500–1000 mg every 4–6 hours, max 3000 mg/day) can be used alone or in combination if NSAIDs are contraindicated.
Stronger opioids are rarely needed; your surgeon will prescribe them only for severe pain and usually for 1–3 days. If prescribed, take the lowest effective dose for the shortest time and avoid driving or mixing with alcohol. Report any adverse reactions or signs of allergy immediately.
If your provider recommends a topical anesthetic or prescription mouth rinse, use it exactly as directed to control localized discomfort and reduce bacterial load.
When to Consult Your Dentist
Contact your dentist if pain worsens after 48–72 hours instead of steadily improving. Increasing pain often signals infection, a failed suture, or other complications that require evaluation.
Seek urgent care for persistent heavy bleeding unresponsive to firm pressure after 20–30 minutes, sudden swelling that makes breathing or swallowing difficult, or high fever (>101.5°F / 38.6°C). These are signs of serious complication.
Report unusual sensations such as numbness or tingling that begin after the initial numbness from anesthesia wears off or that do not gradually improve. These can indicate nerve irritation and may need immediate assessment.
If you notice pus, a bad taste that doesn’t go away, or implant mobility, schedule an appointment promptly. Early intervention improves the chance of resolving problems without implant loss.