Table of Contents
ToggleIf you have lost many teeth, struggle with loose dentures, or want a long-term fix for chewing and smiling, full mouth dental implants can be the solution. Full mouth implants replace an entire upper or lower arch with permanent, strong teeth that look and work like natural ones.
You will learn who makes a good candidate, what the treatment involves, and what results and recovery look like. This guide will help you weigh costs, benefits, and next steps so you can decide if full mouth implants fit your life and goals.
Understanding Full Mouth Dental Implants
Full mouth dental implants replace all teeth in one or both jaws using titanium posts and fixed or removable prostheses. They restore chewing, speech, and facial support, but require surgery, healing time, and good jawbone health.
What Full Mouth Dental Implants Are
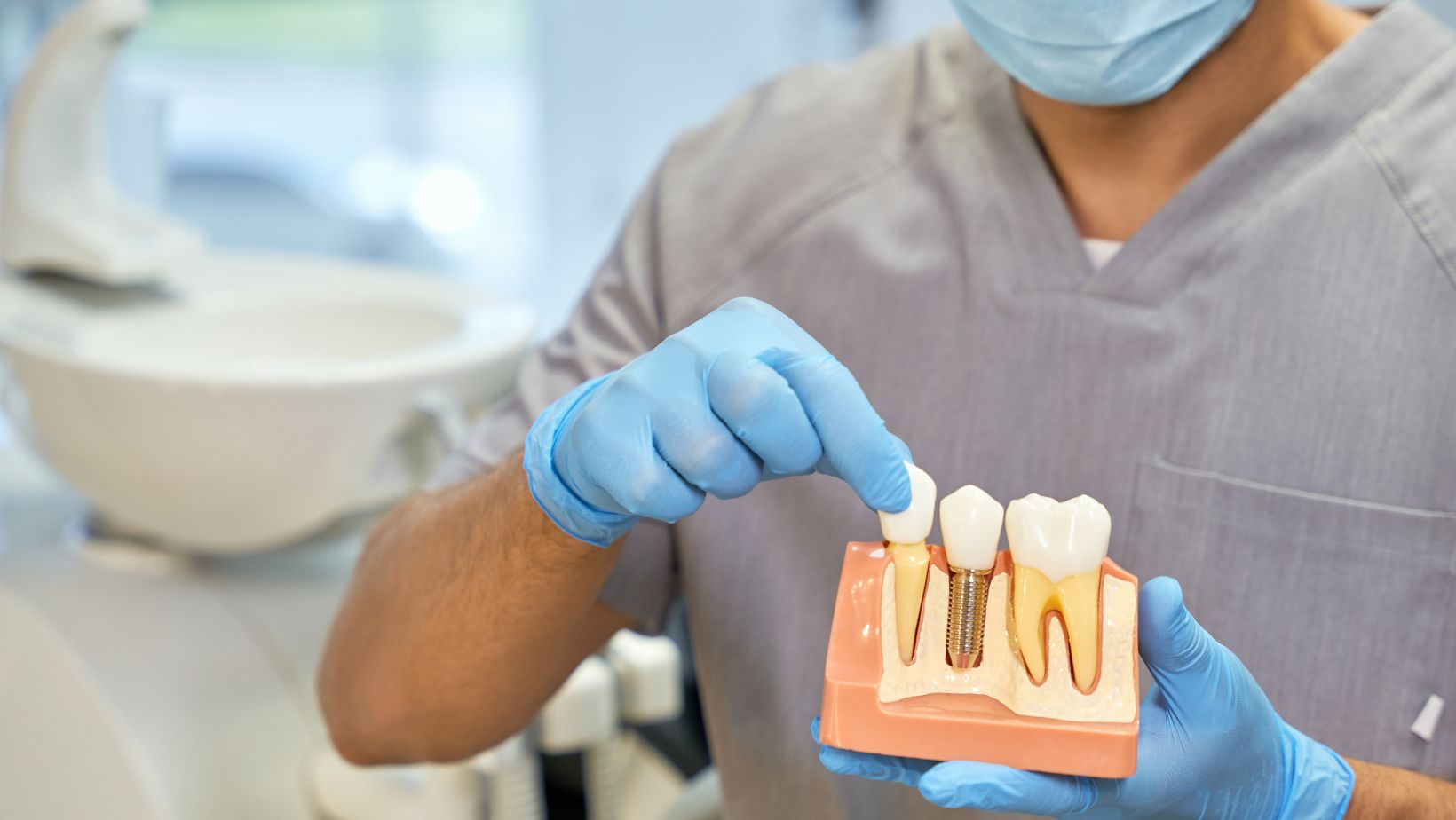
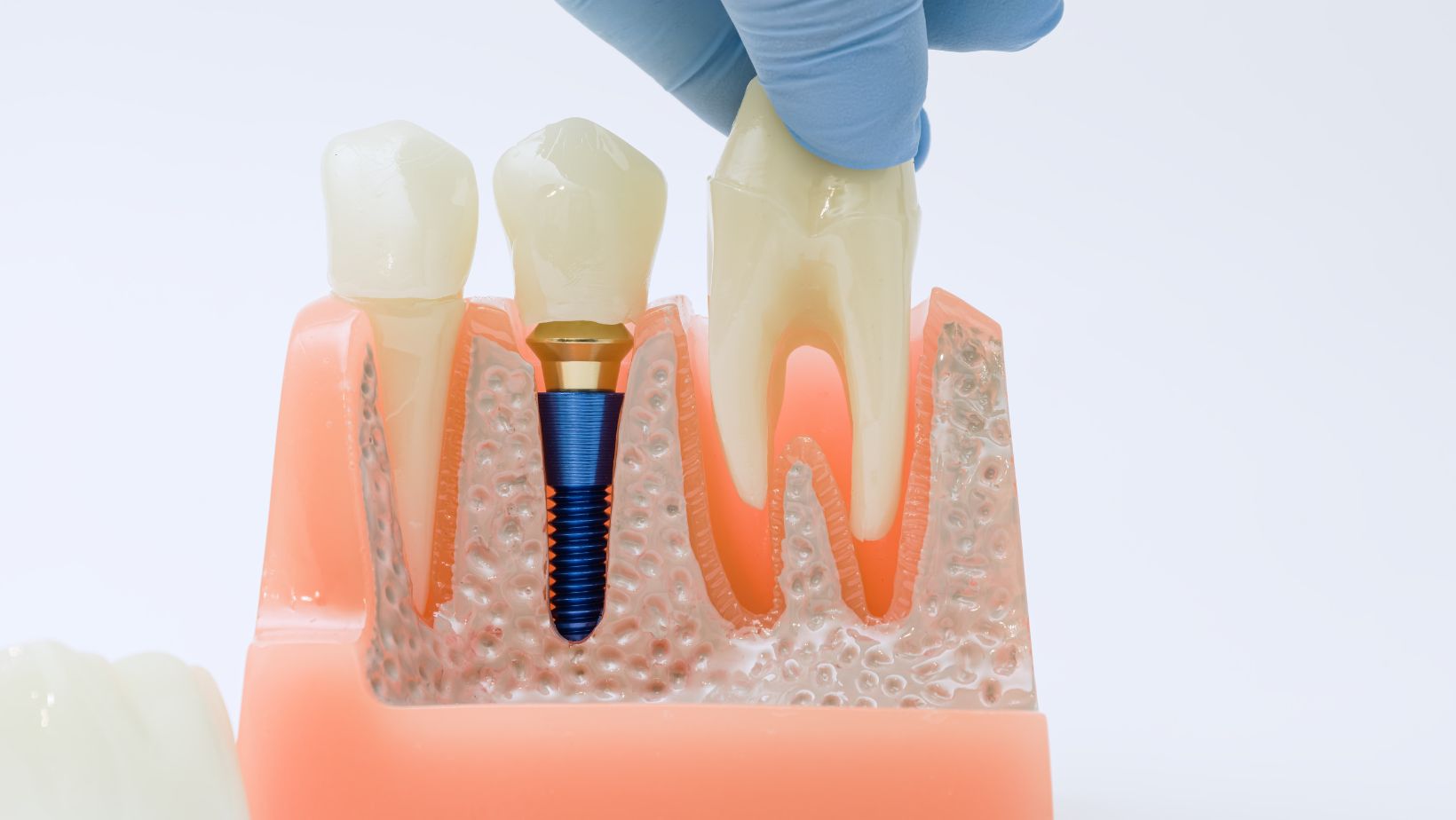
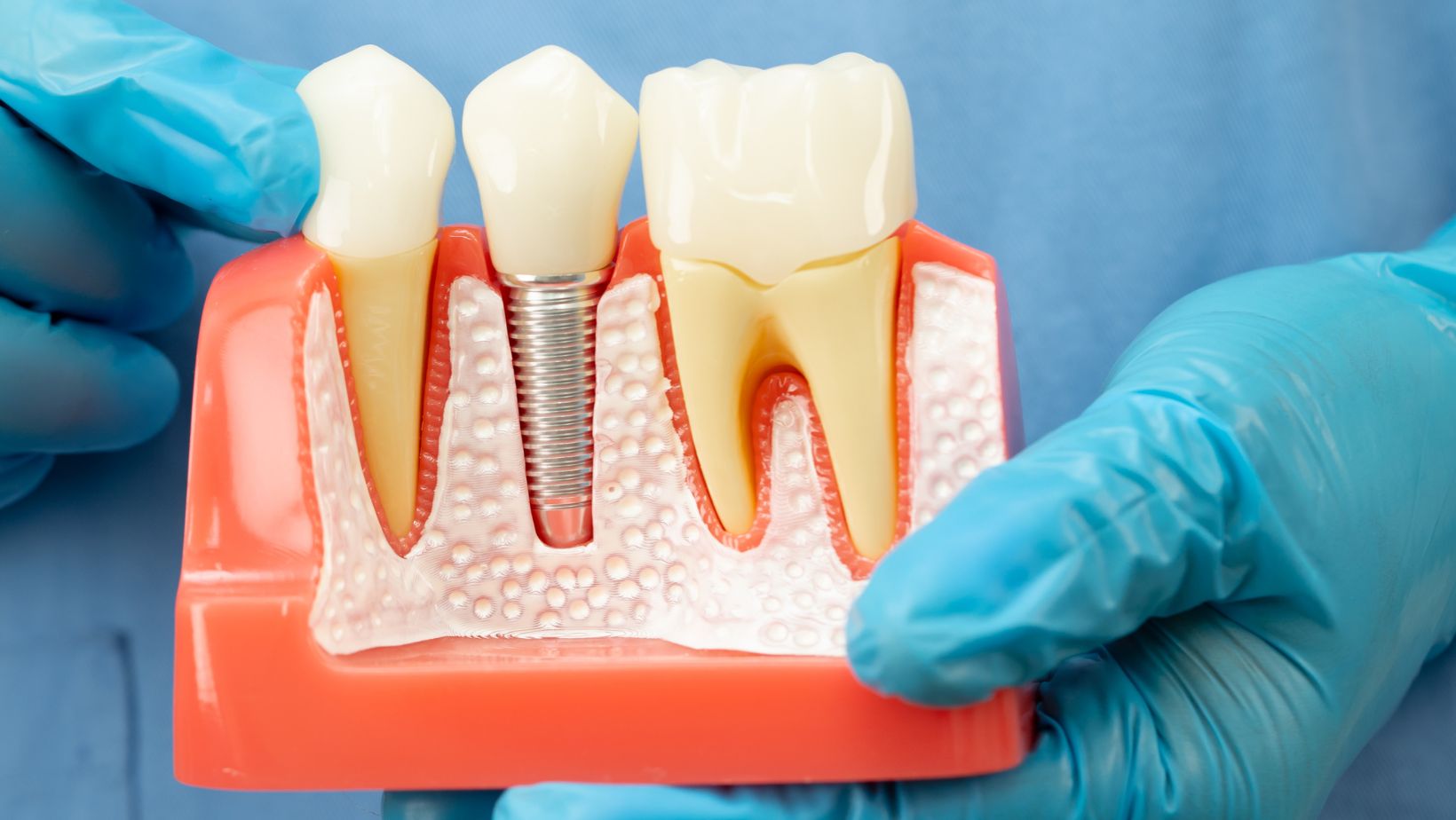
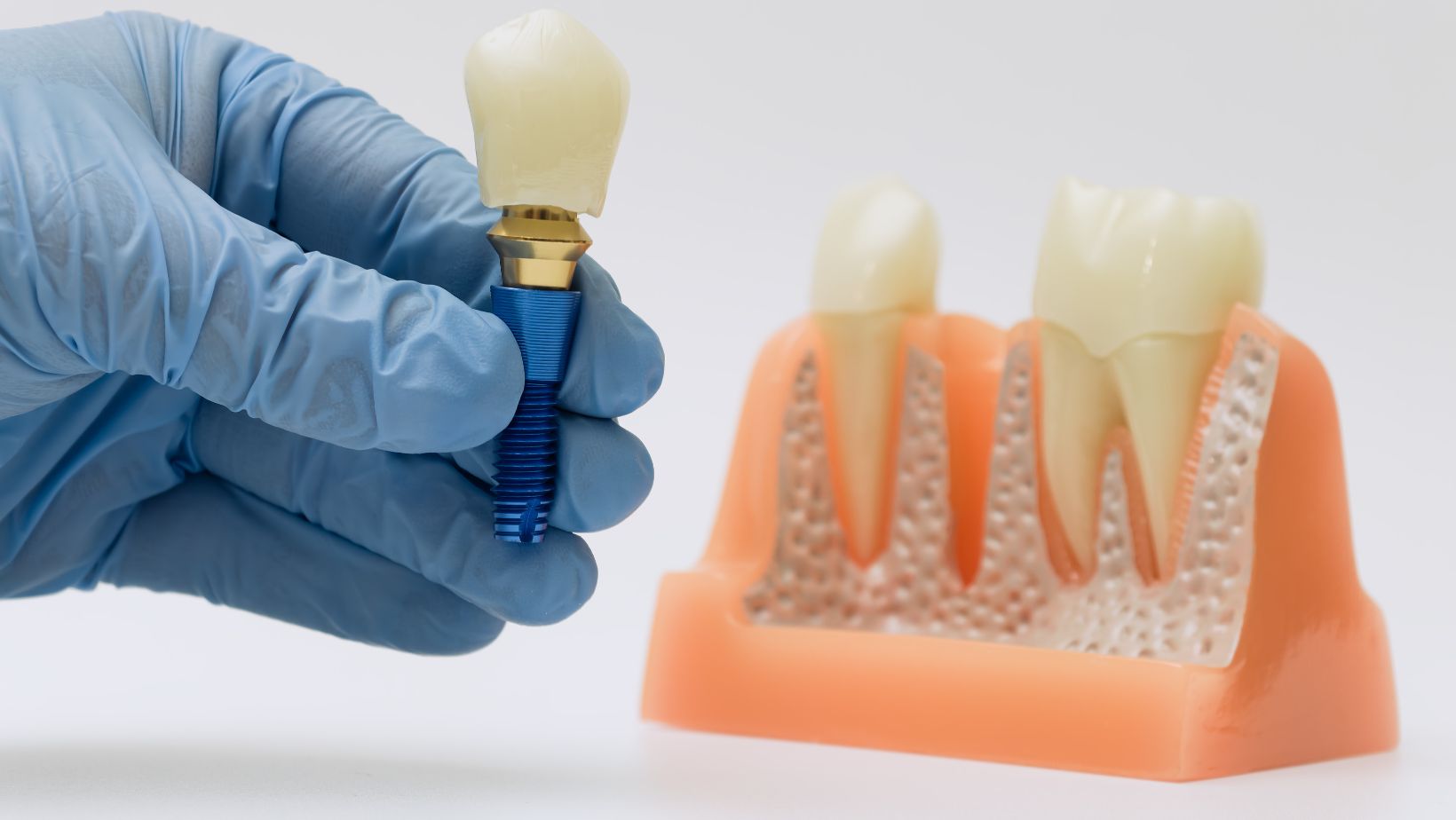
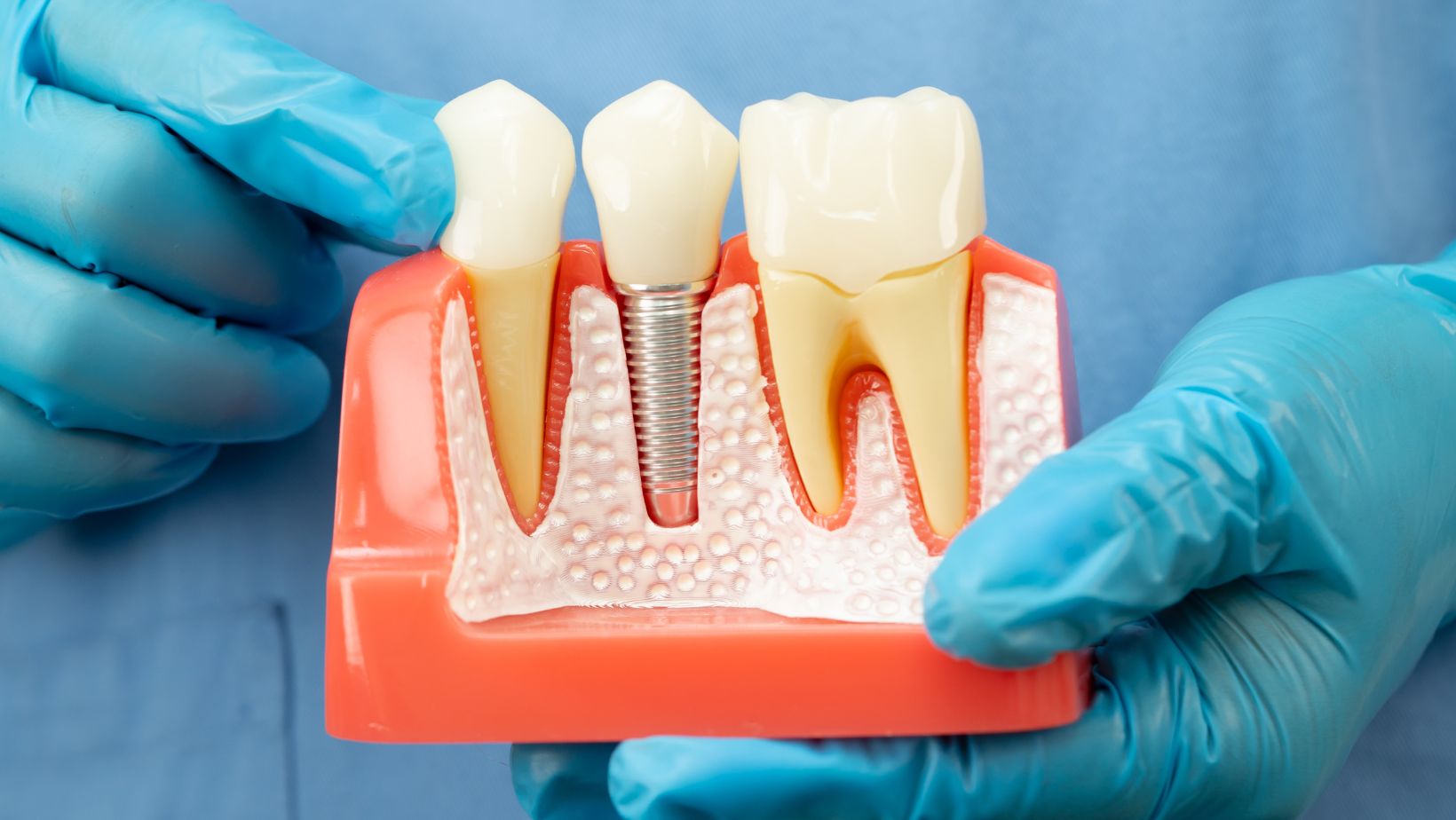
Full mouth dental implants replace every tooth in an upper arch, lower arch, or both. Your dentist places titanium posts into the jawbone to act as artificial tooth roots. After these fuse with bone, a bridge or denture attaches to the posts.
You can get a fixed bridge that you cannot remove, or an overdenture that snaps on and off. Implants look and work more like natural teeth than traditional dentures. They also help stop bone loss by transferring chewing forces to the jaw.
How the Procedure Works
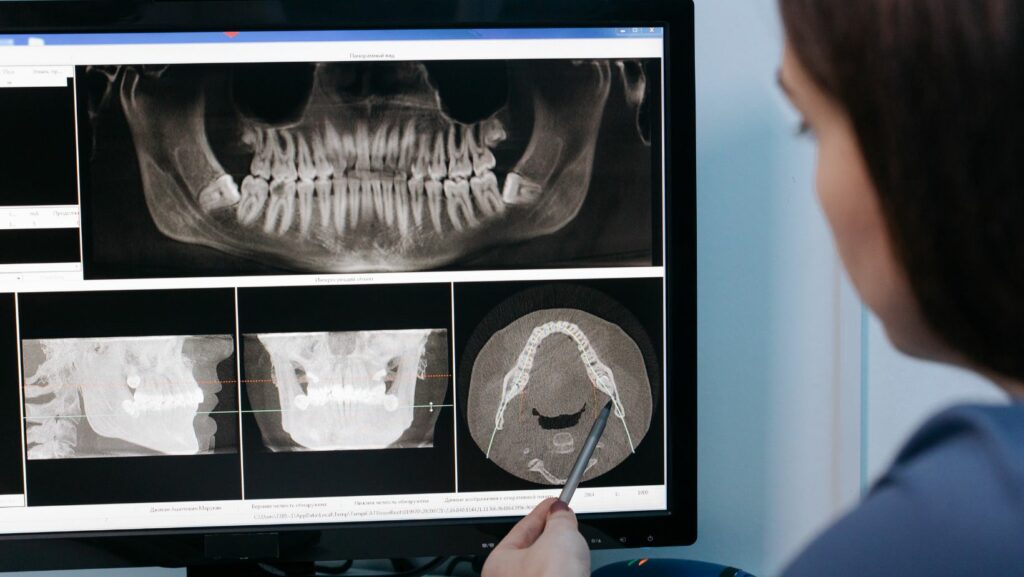
First, your dentist evaluates your mouth with X-rays or a CT scan to check bone volume and plan implant placement. You may need extractions or bone grafts before implants go in. Surgery places implants into the bone, usually under local anesthesia with optional sedation.
After placement, osseointegration takes several weeks to months while the bone bonds to the implants. Your dentist then attaches abutments and fits the final prosthesis. Expect follow-up visits for adjustments and to monitor healing. You will learn daily cleaning steps to keep implants healthy.
Types of Implant Solutions
Fixed full-arch bridges use four to eight implants per arch for a permanent prosthesis you don’t remove. The “All-on-4” approach commonly uses four implants with two tilted posts to avoid bone grafts. This can shorten treatment time.
Removable implant-supported overdentures snap onto two to six implants and cost less upfront. They give better stability than conventional dentures but still come off for cleaning. Your choice depends on bone levels, budget, health, and the level of permanence you want.
Ideal Candidates for Full Mouth Dental Implants
You should have enough jawbone, healthy gums, and stable overall health to heal after surgery. Age alone doesn’t disqualify you; lifestyle, bone quality, and medical conditions matter most.
Eligibility Criteria
You must be missing most or all teeth in an arch or have teeth that cannot be saved. Dentists commonly use All‑on‑4 or All‑on‑6 techniques, placing 4–6 titanium posts per arch to support a fixed prosthesis.
A recent CBCT scan is usually required to measure bone volume and nerve locations. If your jawbone is thin, you may need bone grafting or angled implants; some clinics offer same‑day fixed teeth if bone quality allows.
Financial and time factors also matter. Full mouth implant treatment typically involves multiple visits, imaging, surgery, and healing time. Ask about total costs, warranties, and whether a temporary set of teeth is provided during healing.
Dental Health Considerations
Healthy gums are essential. Active gum disease must be treated first because infection raises the risk of implant failure. Your dentist will check for decay, abscesses, and root infections and remove any hopeless teeth before implant placement.
You should commit to daily oral hygiene and regular dental visits after implants. Brushing, flossing, and professional cleanings keep implants healthy. Smoking and heavy alcohol use reduce healing and raise complication rates; quitting improves outcomes.
Medical Factors Affecting Suitability
Stable general health helps you heal. Conditions like uncontrolled diabetes, recent cancer treatment, or autoimmune disease can slow bone healing and raise infection risk. Your dentist will coordinate with your physician if you have these conditions.
Medications such as bisphosphonates or long‑term steroids can affect bone remodeling. Blood clotting disorders and certain heart conditions require medical clearance. Be ready to share your full medical history and current medications so your dental team can plan safe care.
Expected Outcomes and Benefits
You can expect major improvements in how your teeth look, feel, and work. Many patients regain strong biting power, a natural-looking smile, and easier daily care.
Transformation of Smile and Function
Full mouth implants replace missing or failing teeth with fixed prosthetics that match your tooth shape, size, and color. This gives you a consistent, natural-looking smile that does not shift or lift like dentures.
Function changes quickly: you will regain most chewing strength and can eat a wider range of foods, including tougher proteins and raw vegetables. That helps with nutrition and enjoyment of meals.

Speech often improves because implants stay steady and restore normal tongue and lip support. You won’t need adhesives, and you can speak confidently without worrying about slipping. You may notice small adjustments while you adapt, but those usually resolve in weeks.
Longevity and Durability
Implants use titanium posts that fuse with jawbone, creating a stable base for crowns or bridges. With good home care and routine dental visits, implant-supported prostheses commonly last many years. Individual components like crowns may need replacement after 10–20 years depending on wear.
You should plan for maintenance: regular cleanings, occasional screw or crown checks, and avoiding extreme biting forces. Smoking, uncontrolled diabetes, or poor oral hygiene can shorten implant life, so managing health and habits improves outcomes and durability.
Impact on Oral Health
Full mouth implants help prevent jawbone loss by transmitting bite forces into the bone, which preserves facial structure and supports surrounding teeth. That lowers the chance of further tooth shifting and uneven wear in remaining teeth.
Because implants are fixed, they remove the irritations and sore spots often caused by removable dentures. They also cut down on food traps that can lead to gum disease when hygiene is difficult.
You still need daily brushing and interdental cleaning around implant restorations to prevent peri-implantitis. Regular X-rays and exams let your dentist spot early problems and protect the long-term health of the implants and gums.
Recovery Process and Aftercare
Expect a phased recovery with changing diet, follow-up visits, and gradual return to normal chewing. You will manage pain, protect the implant sites, and watch for signs of infection or implant failure.
Typical Healing Timeline
Days 1–3: You will have swelling, bruising, and bleeding. Use ice packs for 10–20 minutes on/10–20 minutes off during the first 24 hours. Take prescribed pain meds and antibiotics exactly as directed.
Week 1–2: Sutures may dissolve or be removed. You should eat soft foods only and avoid chewing on the implant sites. Light activity is fine, but avoid heavy lifting or vigorous exercise.
Weeks 6–12: Soft bone healing and gum shaping continue. Your dentist checks integration and may allow firmer foods. You often switch from temporary prosthetics to more stable interim teeth.
3–6+ months: Bone integration (osseointegration) completes for most patients. Final prosthetic teeth are placed once your clinician confirms stable implants.
Post-Procedure Care Recommendations
Follow medication and oral hygiene instructions your dentist gives you. Rinse with a saltwater solution (1/2 teaspoon salt in 8 oz warm water) 2–3 times daily after 24 hours to keep sites clean without disturbing healing.
Diet: Stick to soft foods like yogurt, mashed potatoes, and smoothies for 1–4 weeks depending on your surgeon’s advice. Avoid nuts, hard candy, and biting directly on the implants until cleared.
Oral care: Brush gently around implant areas with a soft toothbrush. Use interdental brushes or water flosser once the gum tissue has started to heal, as recommended by your clinician.
Activity: Rest for 48–72 hours and avoid strenuous exercise for at least one week. Sleep with your head elevated the first few nights to reduce swelling.
Follow-up: Attend all scheduled checkups for suture removal, x-rays, and progress checks. Report unusual pain, prolonged bleeding, or loose components immediately.
Potential Risks and Complications
Infection: Watch for increasing redness, swelling, pus, or fever. An infection may need antibiotics or surgical cleanout.
Failure to integrate: If implants do not fuse with bone, they can become loose. Smoking, uncontrolled diabetes, and poor bone quality raise this risk.
Nerve or sinus issues: You may feel numbness, tingling, or sinus pressure if an implant is placed near nerves or the sinus cavity. Notify your dentist immediately if you notice persistent numbness or worsening sinus symptoms.
Prosthetic problems: Screws can loosen, or prosthetic teeth can fracture. Attend maintenance visits and report any mobility, clicking, or pain around the prosthesis.
Follow your clinician’s directions to lower these risks and improve your chance of a stable, long-lasting result.