Table of Contents
ToggleIf you have severe bone loss in your upper jaw and were told traditional implants aren’t an option, zygomatic and pterygoid implants can give you a stable, long-term foundation without extensive bone grafting. These implants anchor into denser bones—the cheekbone or the back of the upper jaw—so you can get fixed teeth when standard implants won’t work.
You will learn how these Zygomatic implants in Wisconsin differ, why surgeons choose one over the other, what the surgery involves, and what outcomes to expect. The article covers clinical steps, recovery factors, and real patient benefits so you can decide if this advanced approach fits your needs.
Understanding Zygomatic and Pterygoid Dental Implants
These implants use stronger bones outside the atrophied upper jaw to support fixed prosthetic teeth. They let you get stable implants without bone grafts in many cases.
Definition and Anatomy
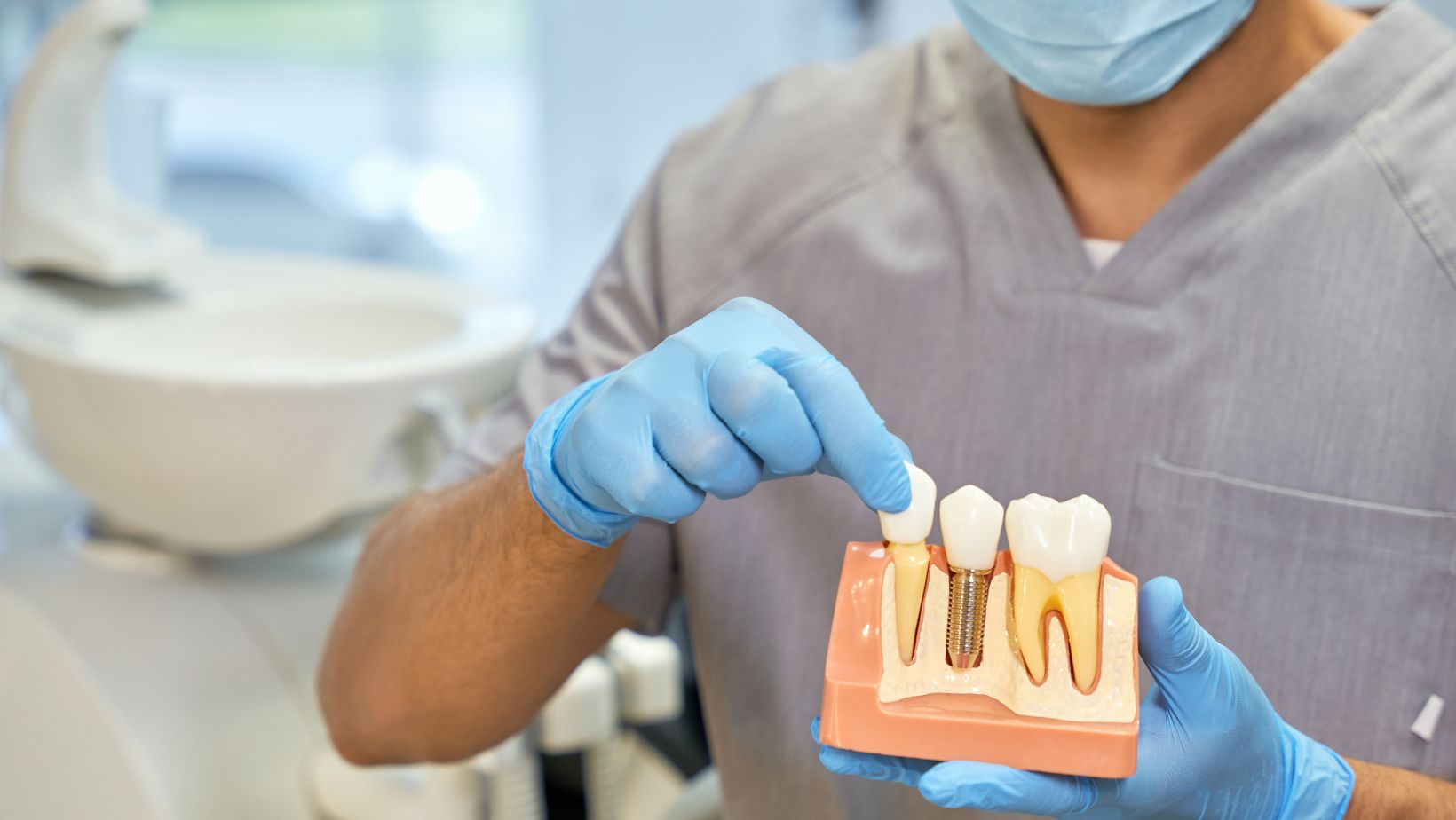
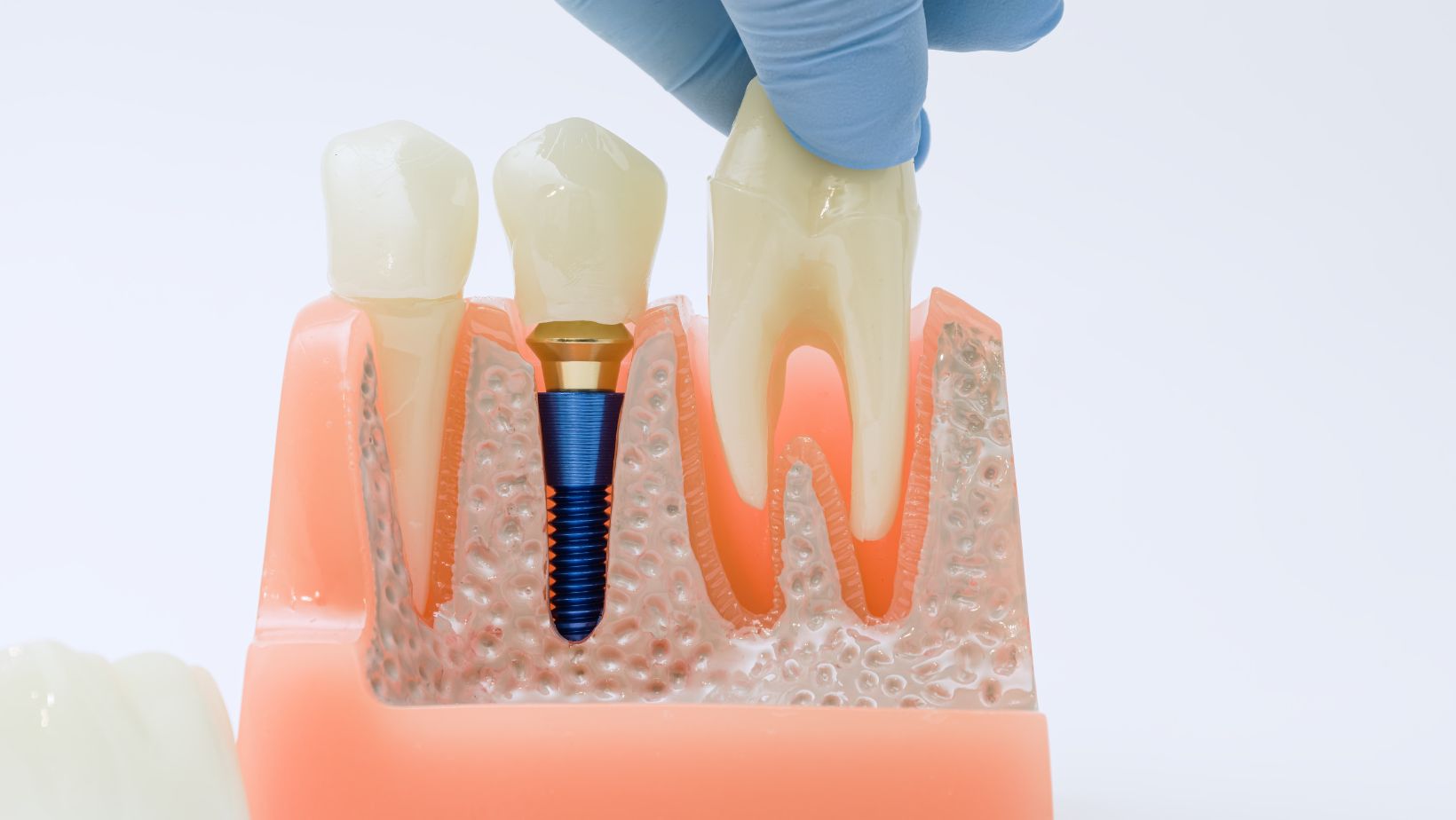
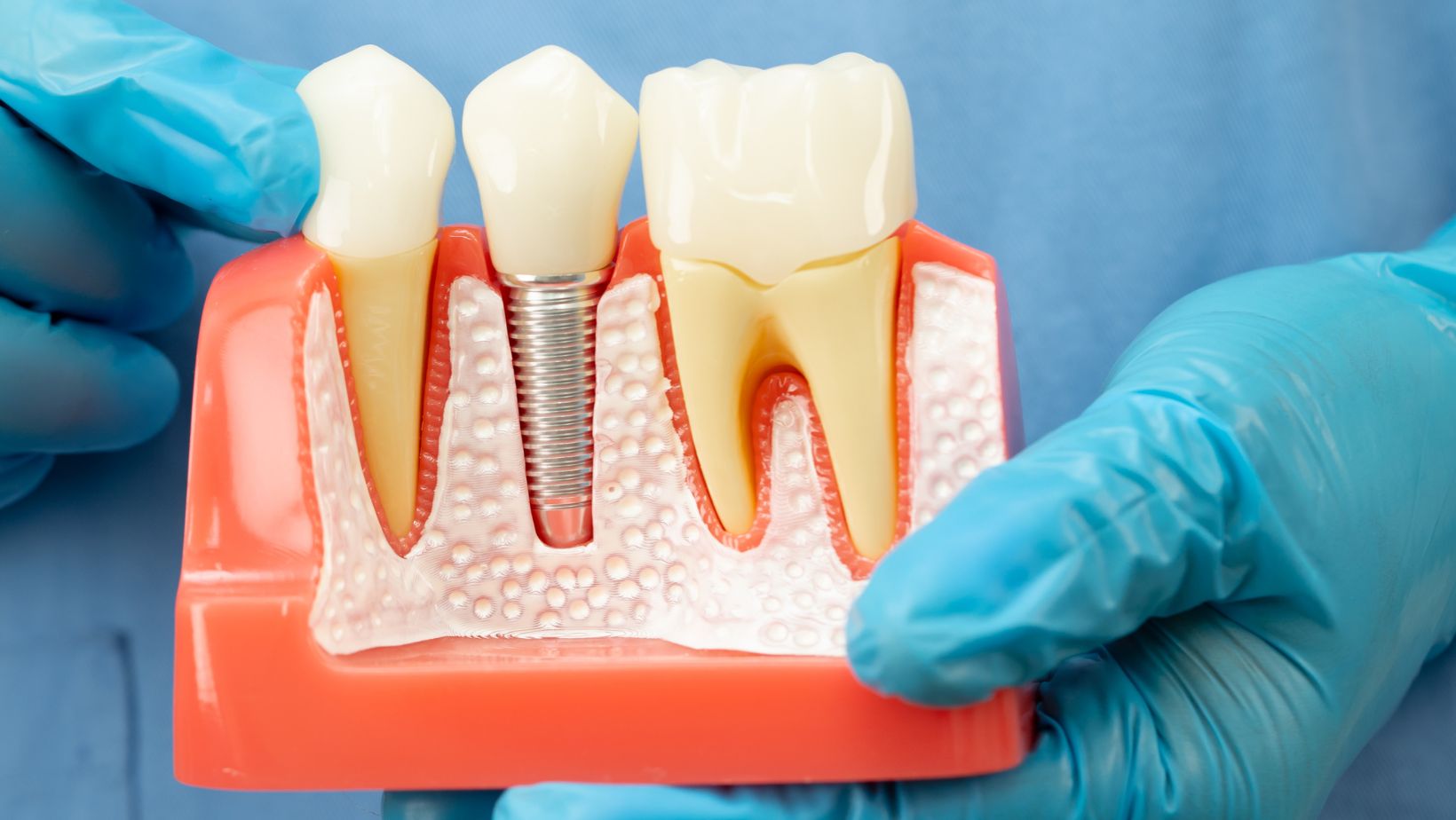
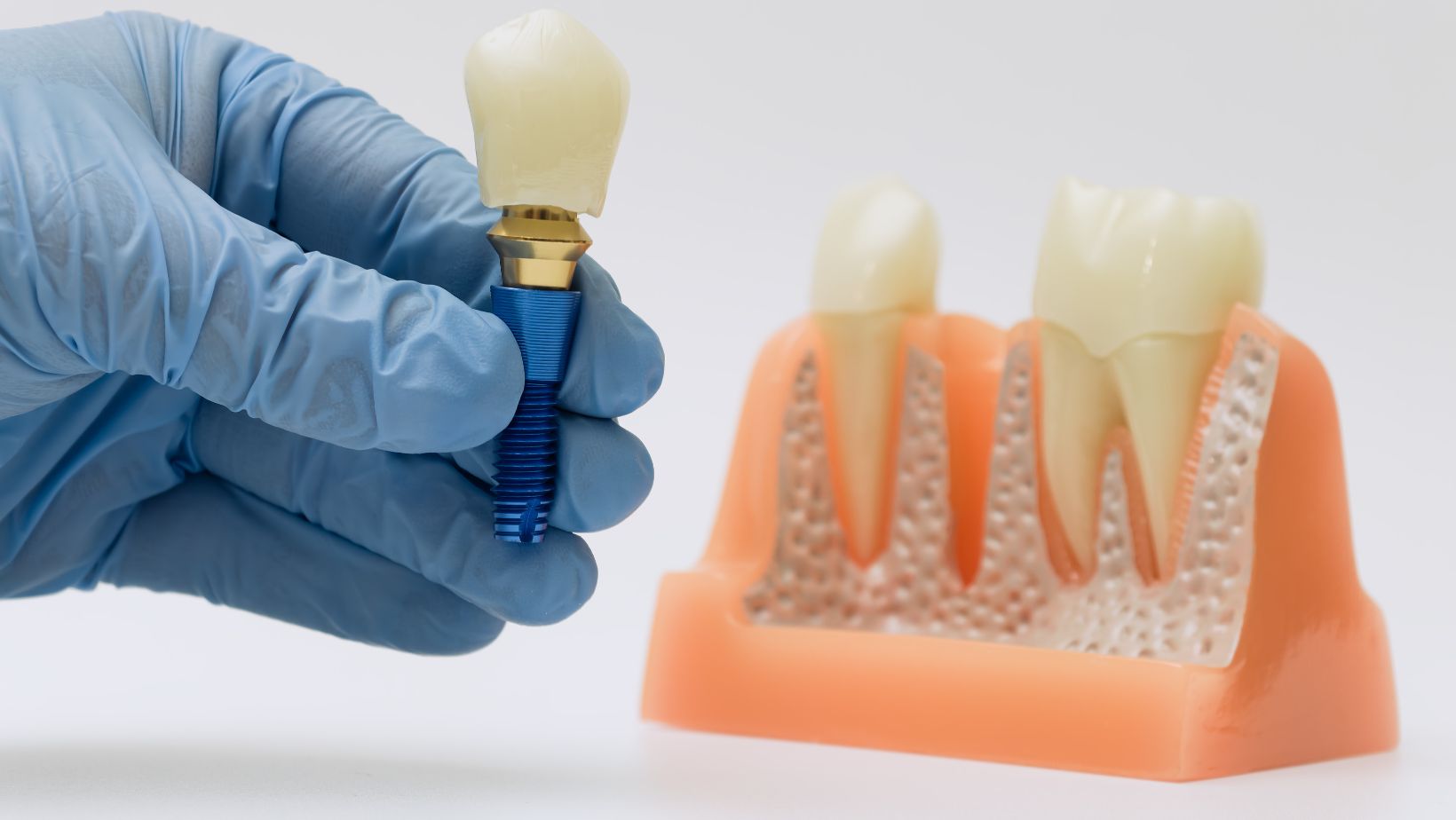
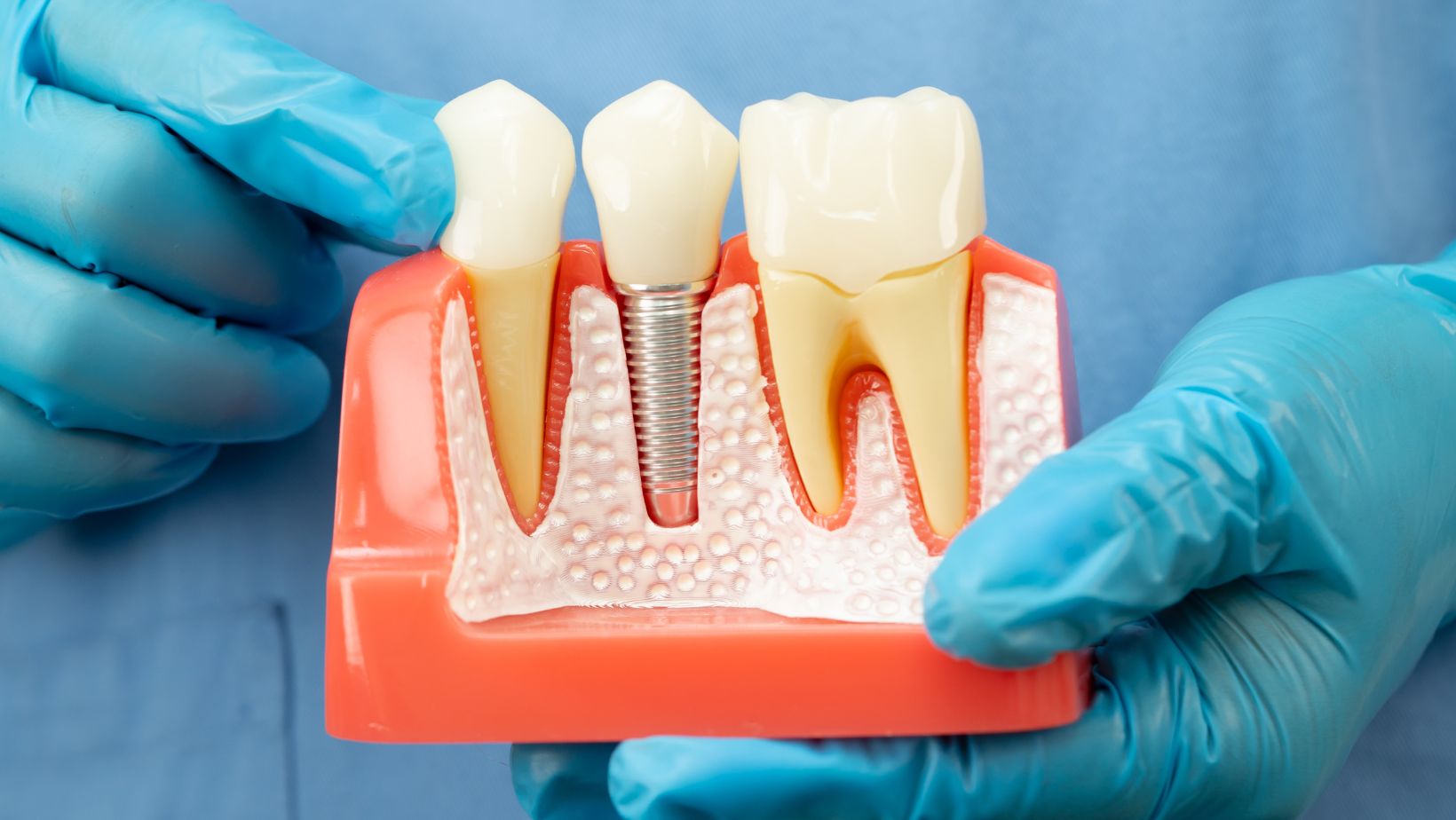
Zygomatic implants are long screws anchored into the zygomatic bone (cheekbone). The zygoma is dense and thick, which gives strong support when the upper jaw (maxilla) has lost bone volume.
Pterygoid implants are placed toward the back of the upper jaw and engage the pterygoid plate of the sphenoid bone. That plate is also dense and avoids the sinus cavity in many placements.
Both implant types are longer than standard implants and follow an angled trajectory. This trajectory matters for surgical planning and prosthetic design.
Comparison to Traditional Dental Implants
Traditional implants sit in the alveolar bone of the jaw where your natural teeth used to be. They need enough bone height and width. When bone is missing, clinicians usually consider bone grafting, sinus lifts, or short implants.
Zygomatic and pterygoid implants bypass the need for grafting by anchoring into alternative bones. They require different surgical access, angled prosthetic components, and precise imaging like CBCT scans. Healing and loading protocols can still allow immediate or early loading in many cases.
Indications for Use
You may be a candidate if you have severe maxillary bone loss from periodontal disease, long-term denture wear, trauma, or congenital defects. They suit people who cannot or prefer not to undergo bone grafting or multiple staged surgeries.
They also fit patients needing full-arch fixed prostheses when posterior bone is deficient. Not every patient qualifies; adequate systemic health, controlled gum disease, and careful evaluation of sinus anatomy and facial bone structure are required.
Advantages Over Conventional Options
You avoid lengthy grafting procedures and the months of healing they require. That often reduces total treatment time and the number of surgeries.
You get access to denser bone for primary stability, which can increase the chance of immediate or early loading of a prosthesis. This means you can receive fixed teeth faster.
These implants also expand treatment for patients previously told they were not candidates for implants. However, they demand advanced surgical skill and careful planning to manage risks like sinus involvement or nerve proximity.
Addressing Severe Bone Loss with Advanced Implant Solutions
You will learn how limited bone affects implant options, what tests confirm suitability, and how a tailored plan uses zygomatic or pterygoid implants to restore stable teeth.
Challenges of Severe Maxillary Bone Loss
Severe bone loss in the upper jaw removes the usual support for standard implants. You may lack height and density in the posterior maxilla, and the sinus can encroach on the implant site. This makes short implants unstable and increases the risk of failure.
Sinus lift or bone grafting can add months of healing and may still not provide predictable support for traditional implants. Zygomatic and pterygoid implants avoid grafts by anchoring into the cheekbone or pterygoid plates, where bone is denser. That anchorage offers immediate stability and lets you receive fixed teeth faster than staged grafting approaches.
Candidacy Evaluation and Diagnostics
Your clinician will take a detailed health history, including smoking, diabetes, and medications that affect bone healing. These factors change success rates and treatment choices.

A cone beam CT (CBCT) scan maps your anatomy in 3D. The scan shows zygoma thickness, sinus position, and pterygoid plate orientation. Physical exam checks soft tissue quality and mouth opening. Together these steps determine whether zygomatic or pterygoid implants suit you, or if alternative solutions are safer.
Customized Treatment Planning
Planning starts with a digital surgical guide based on your CBCT and intraoral scans. Your surgeon selects implant length, angulation, and number to reach dense bone while avoiding nerve and sinus damage. That plan also defines whether one or both sides need zygomatic or pterygoid anchorage.
Your restoration timeline gets set: same-day fixed provisional teeth or staged prosthetics. The plan includes anesthesia type, postoperative care, and contingency for complications. Clear written consent outlines risks, benefits, and costs so you know what to expect at each step.
Surgical Techniques and Clinical Considerations
You will learn how surgeons place zygomatic and pterygoid implants, what to watch for during surgery, common complications, and how recovery is managed. The focus is on exact placement steps, anatomical landmarks, patient safety, and post-op care.
Placement Procedures for Zygomatic Implants
Zygomatic implants anchor in the cheekbone (zygoma) when the upper jaw lacks bone. Your surgeon begins with a CT-based plan to map the zygoma’s thickness and the implant trajectory.
Incisions typically expose the alveolar crest and zygomatic buttress. Drill sequence follows a planned angulation to engage dense cortical bone of the zygoma while avoiding the orbit and infraorbital nerve.
You may get either an intrasinus or extra-sinus approach depending on sinus anatomy. The intrasinus route passes through or alongside the maxillary sinus; the extra-sinus route stays lateral to the sinus. Screws are long (often 30–55 mm) and must achieve primary stability in cortical zygomatic bone.
Surgeons often use guided templates or navigation for accuracy. You should be informed about planned implant length, angulation, and whether simultaneous immediate loading (temporary teeth same day) is intended.
Pterygoid Implant Technique Overview
Pterygoid implants anchor in the pterygoid plate region behind the maxillary tuberosity to gain posterior support. You will receive imaging to confirm the tuberosity and pterygoid canal anatomy. The entry point is usually at the tuberosity crest or slightly posterior.
Your surgeon angles the drill about 45–70 degrees posteriorly and medially to follow the pterygoid pillar toward dense cortical bone. The implant length typically ranges 14–20 mm or longer depending on bone depth. Primary stability is critical since these implants often support distal occlusion without grafting.
Soft-tissue management aims to keep the mucosa intact or close the site to prevent food impaction. You should understand how the implant trajectory avoids the greater palatine neurovascular bundle and the pterygoid venous plexus.
Potential Risks and Complications
You face risks common to advanced implants plus some unique to these sites. Expect possible sinusitis, oro-antral communication, infraorbital or greater palatine nerve irritation, and bleeding from the pterygoid plexus. Orbital injury risk is extremely low but serious, so careful angulation matters.
Other complications include implant malposition, insufficient primary stability, and prosthetic misfit if trajectories differ between sides. Infection or soft-tissue dehiscence can expose implants. Smoking, uncontrolled diabetes, or prior radiation increase complication risk.
Surgeons reduce risk by using CBCT planning, surgical guides, careful hemostasis, and staged approaches when bone or soft tissue looks compromised. Ask about contingency plans, like sinus repair or staged loading, before surgery.
Recovery and Post-Operative Care
Expect swelling, bruising, and mild to moderate pain for several days. Your surgeon will prescribe antibiotics and analgesics and may recommend nasal decongestants if the sinus was involved. Keep your head elevated and avoid nose-blowing for at least two weeks when sinus work occurred.
You must follow a soft diet for 2–6 weeks depending on loading. Attend follow-up visits at 1 week, 2–4 weeks, and then monthly until prosthesis delivery. Maintain oral hygiene with gentle rinses and avoid mechanical trauma to the surgical sites.
Report persistent facial numbness, severe pain, heavy bleeding, fever, or signs of implant mobility immediately. If you smoke, stop before and after surgery to improve healing and implant success.
Long-Term Outcomes and Patient Benefits
Zygomatic and pterygoid implants often give durable support, restore chewing and speaking, and reduce the need for bone grafts. They can work when your upper jaw lacks sufficient bone and can let you get fixed teeth faster than grafting.
Success Rates and Longevity
Studies show zygomatic and pterygoid implants have high survival rates over 5–10+ years when placed by experienced clinicians. You can expect implant survival commonly reported above 90% in many series, though exact rates vary with patient health and surgical technique.
Peri-implant infection and sinus-related issues are the main biological risks to monitor. Regular follow-up and hygiene reduce those risks and help implants last. Your surgeon’s skill, prosthesis design, and how well you maintain oral care influence long-term stability.
Documented prosthetic survival is also strong; bridges and full-arch prostheses supported by these implants often function for many years with routine maintenance and occasional repairs.
Functional and Aesthetic Improvements
You will regain bite force needed for most foods, improving nutrition and meal enjoyment. These implants anchor into denser facial bones, giving a stable base for fixed bridges rather than removable dentures.
Fixed prostheses restore tooth height and facial support, which helps lip contours and reduces sunken appearance. Aesthetics depend on prosthesis design and shade selection; good planning delivers natural-looking teeth that match your smile line.
Speech often improves because the prosthesis stays in place. That stability cuts down on slippage and clicking that you might have had with dentures.
Quality of Life Enhancements
Many patients report immediate emotional relief from having fixed teeth instead of removable dentures. You will likely feel more confident in social settings and less anxious about prosthesis movement.
Daily life changes include easier eating, simpler hygiene routines compared with frequent denture care, and fewer clinic visits than complex grafting timelines. Faster rehabilitation often means you return to normal activities sooner.
Keep realistic expectations: maintenance visits, possible repairs, and good oral hygiene remain necessary to protect your investment and long-term comfort.